Dissolving Lip Filler Using Hyaluronidase
As the popularity of aesthetic treatments rise, so too does the rate at which complications occur. This is especially true given the field’s current lack of regulation in the UK and diverse range of treatment providers. As such, dissolving lip filler using hyaluronidase is a technique all injectors should learn.
Dissolving lip filler is a key skill for emergent and elective, more controlled scenarios. Vascular occlusion is an instance where lip filler requires dissolving, as well as less acute circumstances. These include infection or late onset nodules.
Reversing lip filler can also be offered as a correctional service to patients who have experienced poor results. These are the cases where they may choose to have their filler dissolved. This is usually due to an unsatisfactory aesthetic outcome, rather than it being required clinically.
Due to the nature of its use, lip filler training will generally not involve practical experience of treating with hyaluronidase – often referred to by the brand name Hyalase. As such, it can be helpful to acquire as much expert information and guidance as possible.
Experts’ experiences of dissolving lip filler using hyaluronidase
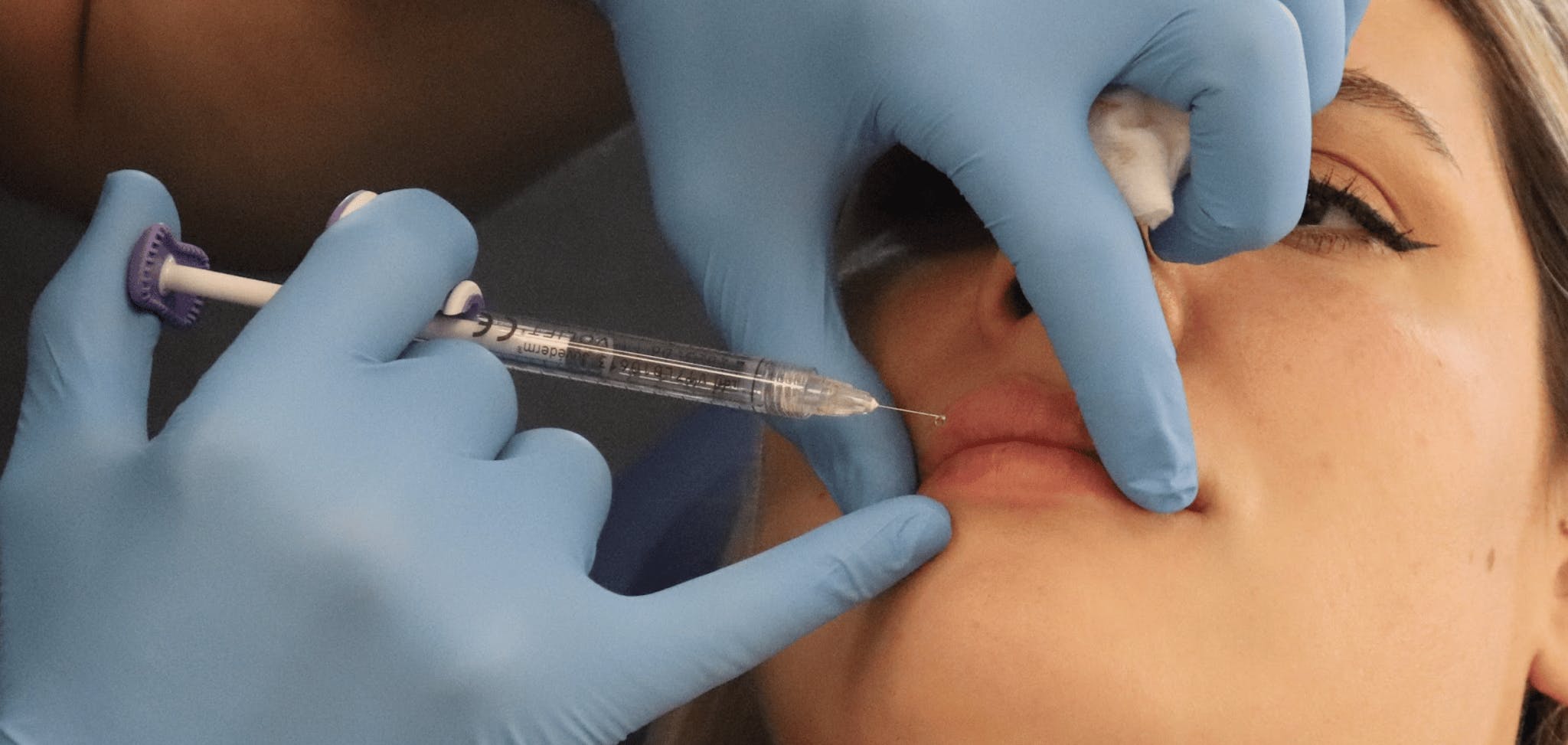
Here three aesthetics specialists share their advice for dissolving lip filler and experiences of using hyaluronidase.
Natalie Haswell (Nat) is a cosmetic nurse prescriber who runs her own CQC-registered clinic, Haswell Aesthetics. She is a senior clinical trainer at Harley Academy and an Allergan Medical Institute faculty member.
Dr Harriet Jenkins is an experienced aesthetics specialist based at Rachel Stagg Aesthetics alongside being a Clinical Lead at Harley Academy. She also has experience as an NHS anaesthetist.
Dr Jess Srivastava is the cosmetic medicine specialist behind Dr Jess Aesthetics. She is a clinical trainer at Harley Academy and is an Allergan Spark award recipient.
Tell us about the first time you dissolved lip filler…
Nat: “The first time I dissolved lip filler was for a lady who had had lip filler elsewhere. It was an elective dissolve, it wasn’t an emergency due to vascular occlusion or anything. The patient wanted to have the product dissolved. During, I was really nervous because there’s a higher risk of allergy with something like hyaluronidase, which is the drug that we use to dissolve temporary fillers. So I was nervous, sometimes it can be a little bit uncomfortable for the patient which doesn’t sit well with me – I don’t want my patients to be in discomfort – but afterwards I was pleased. She was pleased. It went really well, we didn’t have any complications or problems. Once the filler had been dissolved, two months later we re-filled the lips and they looked better and much more natural.”
Dr Harriet: “The first time I dissolved lip filler was an elective procedure for the treatment of migrated filler. The patient was aware that the filler had migrated and it was explained to them that further treatment on top of this would not have a satisfactory outcome. Treatment decisions were discussed and the patient elected to have the filler dissolved. She was subsequently re-treated.”
Dr Jess: “The first time I dissolved filler was for a patient that had lip lumps and had been elsewhere for treatment but lost trust in that practitioner. I had done some other treatments for her in the past so, as an exception to my ‘I don’t dissolve other people’s work’ rule, I felt like I wanted to help her. The reason I don’t like dissolving other people’s work is partly because it’s not a nice experience; it can often be uncomfortable despite numbing cream. After the treatment I could tell the patient was in discomfort throughout but she was grateful to have the lip filler dissolved and we could then refill two weeks later.”
What should injectors be aware of when administering hyaluronidase?

Nat: “When dissolving lip fillers using hyaluronidase there’s a high risk of allergy. If you’re not using lidocaine in the mix then it can be quite uncomfortable for the patient. When you administer it you need to obviously make sure you have taken informed consent that details all of these things. There’s a really good consent form that you can obtain through some complication groups about Hyalase. Just be mindful that giving your patient as much information as you can in advance should prepare and reassure them, make them more comfortable and hopefully it’ll go well.”
Dr Harriet: “The most significant risk to be aware of is allergy. You need to be prepared and ready to treat this, should it arise. Patients need to be suitably consented and aware of this risk. Common risks associated with dissolving filler using hyaluronidase include swelling and bruising, especially in the lips.”
Dr Jess: “As has been mentioned, one of the biggest concerns with dissolving is the chance of an allergic reaction. In a non-emergency situation I would recommend intradermal testing and ensuring no reaction. However, in an emergency situation this wouldn’t be possible. Always have your emergency drugs kit close by and ensure it’s in date.”
What’s your best advice for dissolving lip filler correctly?
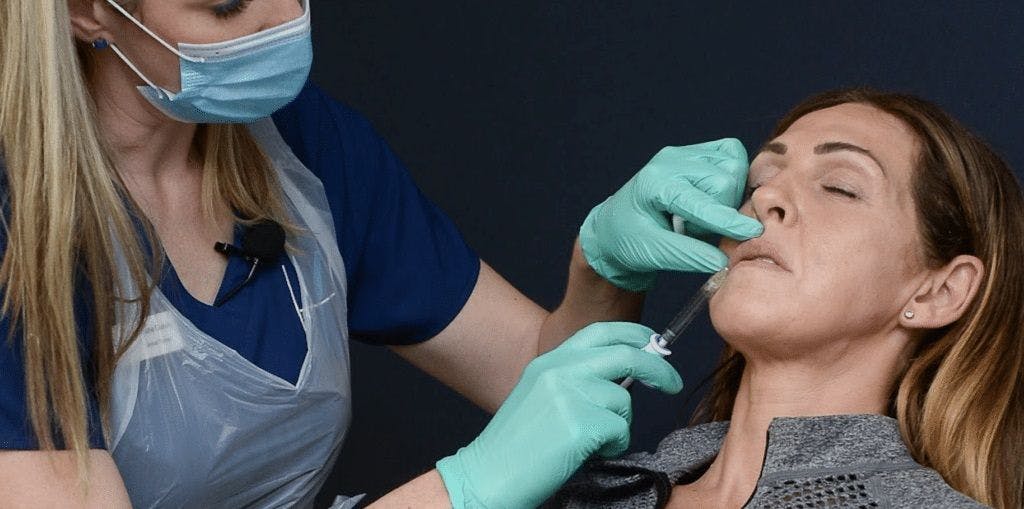
Nat: “Follow the protocols that you can get, again, from some of the complication expert groups. They’re there for a reason. They’re there to help you and based on research, guidance and science so they should be as safe as possible. Take your time – there’s absolutely no rush unless, obviously, there is a vascular occlusion. In that case just make sure you follow the protocol, contact complications groups if needed – I recommend joining one or both of the two really popular groups at the moment, CMAC and ACE Group. Also make sure you have your emergency drugs should you have any complications, such as allergy.”
Dr Harriet: “As Nat says, take your time, follow guidelines for elective dissolving and find a dilution protocol you feel comfortable with. Use the smallest amounts of Hyalase possible during dissolving. Again, take your time, inject small amounts slowly, massage following injection and allow time for the hyaluronidase to work. Repeat until you’re happy.”
Dr Jess: “When dissolving and it’s your work, you know exactly where you have injected and it is easier to retrace your steps with hyaluronidase. When it is someone else’s work it’s difficult as you might also not know what product was used and in which layer it was injected. If you can feel or see filler, ensure that you inject around it and within it and firmly massage. In an emergency situation you would repeat this every 45 minutes until you establish a normal capillary refill.”
What are your tips for patient care in this scenario?
Dr Harriet: “Ensure the patient fully understands what the process involves and what to expect afterwards, this should all be done during the consultation process. Also make sure patients are aware it may take more than one session to fully dissolve depending on the indication and filler used.”
Nat: “Really effective, clear, concise communication. Take your time to consult the patient, especially if it’s elective dissolving. Take the time to consult them, explain everything and answer their questions fully.”
Learning more about lip filler complications
Learning how to prevent, identify and manage complications from dermal filler, including lip fillers, is covered in these aesthetic medicine training courses:
Level 7 Diploma in Botox & Dermal Fillers (in-depth learning).
Foundation Training in Botox & Dermal Fillers (basic overview).
Core Training in Botox & Dermal Fillers (intermediate learning).
Preventing and Managing Dermal Filler Complications (targeted eLearning)
Advanced Complications Management Masterclass (small group in-depth learning, also includes the above eLearning).
These courses are all open to licensed doctors, dentists, nurses and midwives. For specific eligibility requirements or more detailed information, contact Deneal Basi, our head of student recruitment. Together, you can discuss your best options for becoming a safe and knowledgeable aesthetic practitioner who can produce beautiful lip filler results.
All information correct at the time of publication
Download our full prospectus
Browse all our injectables, dermal fillers and cosmetic dermatology courses in one document
By submitting this form, you agree to receive marketing about our products, events, promotions and exclusive content. Consent is not a condition of purchase, and no purchase is necessary. Message frequency varies. View our Privacy Policy and Terms & Conditions
Attend our FREE open evening
If you're not sure which course is right for you, let us help
Join us online or in-person at our free open evening to learn more
Our Partners















STAY INFORMED
Sign up to receive industry news, careers advice, special offers and information on Harley Academy courses and services

