How to tell Eyebrow Ptosis from Lid Ptosis
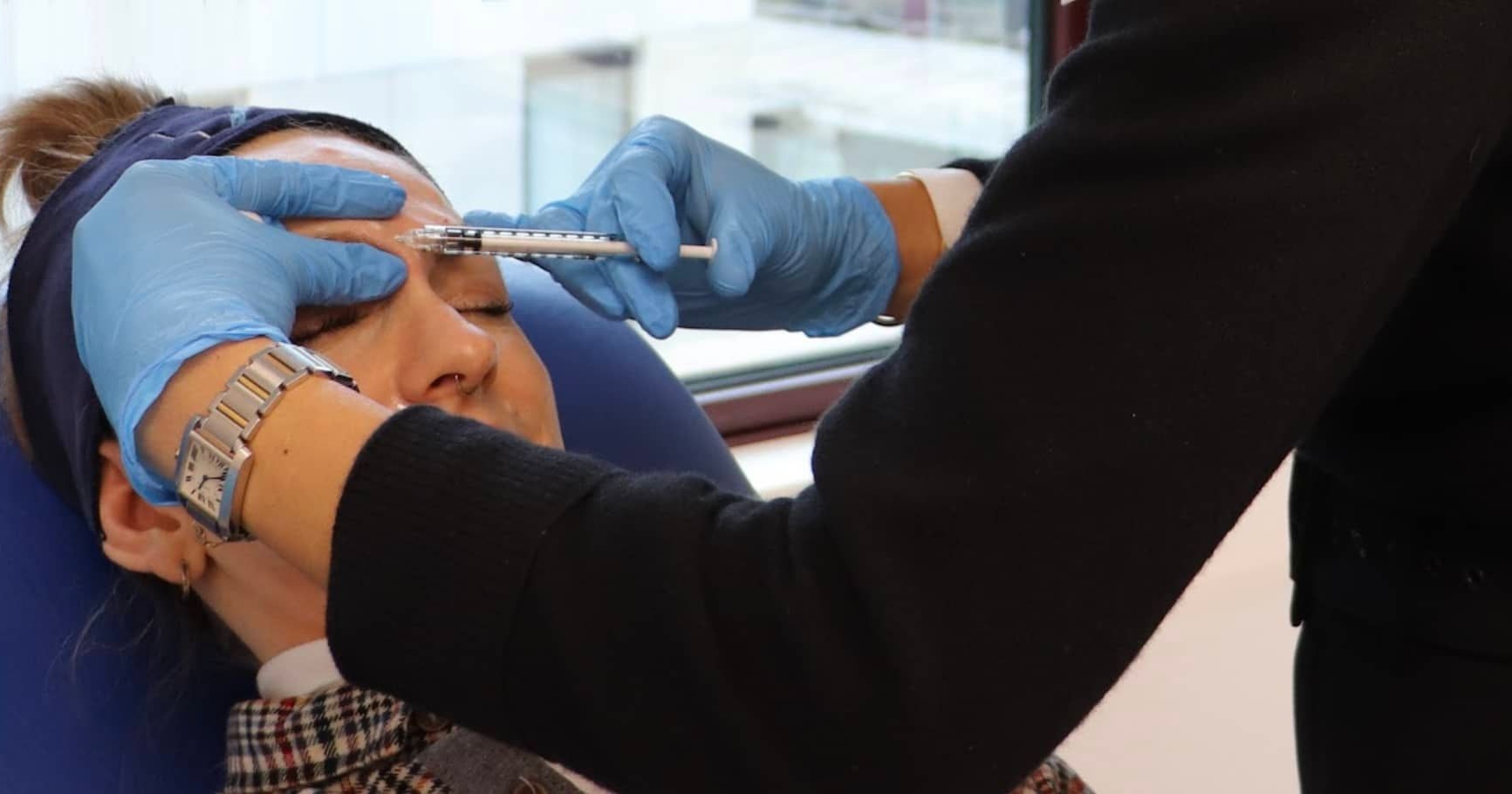
What’s the difference between eyebrow ptosis and lid ptosis? As an aesthetics practitioner, you need to be able to accurately diagnose each of these ptoses.
Dr Kalpna Pindolia is a facial aesthetics specialist and director of education at Harley Academy.
Here she explains how to tell eyebrow ptosis from lid ptosis and what causes these complications. She also provides tips on how to correct these ptoses, where possible...
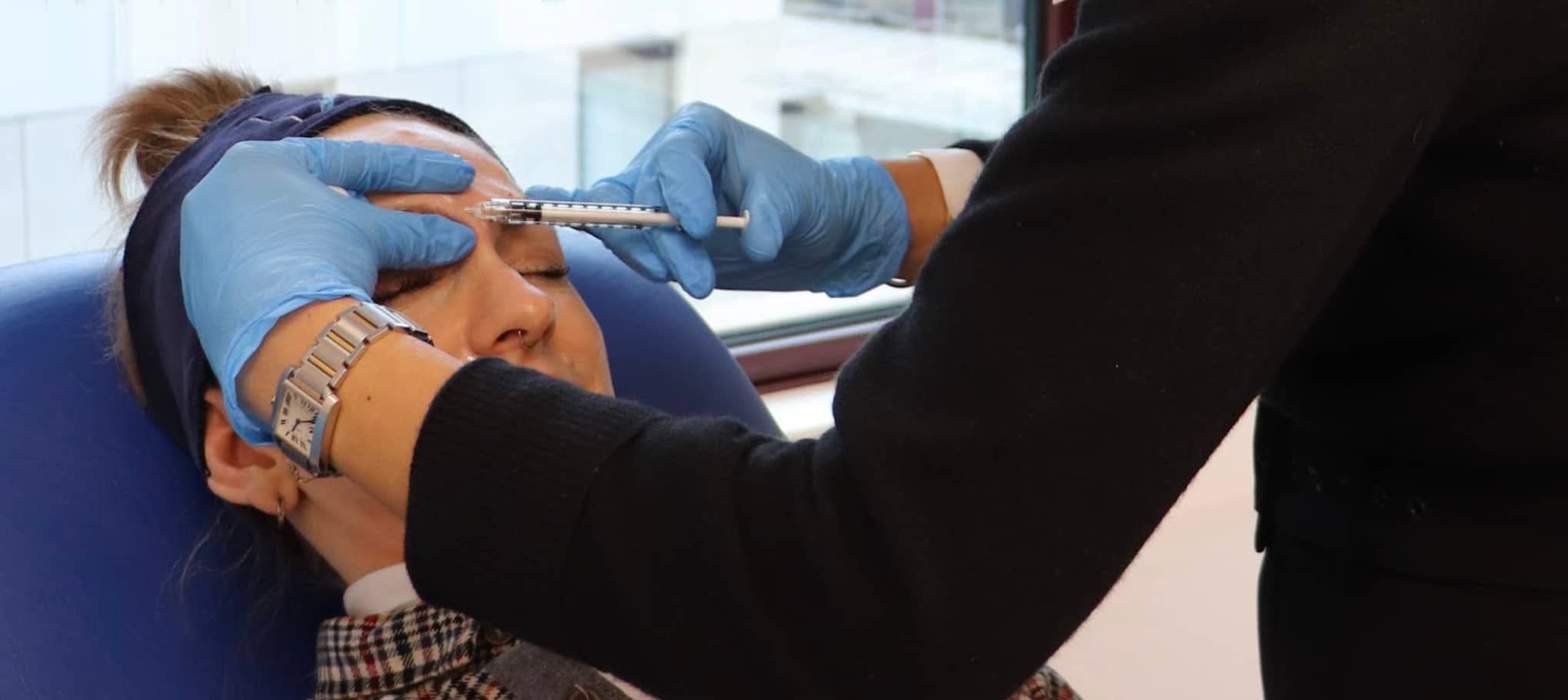
WHAT IS PTOSIS?
“Ptosis refers to the drooping or abnormal lowering of an anatomical area,” explains Dr Kal.
“In the eye region, botulinum toxin complications of eyelid or eyebrow ptosis can cause a displeasing facial aesthetic. They can also cause functional issues, such as visual field compromise, eye strain or ache. It’s important to know whether you’re treating upper eyelid or eyebrow ptosis as the causes and management are different.”
GENERAL PTOSIS CONSIDERATIONS
Dr Kal recommends you understand the following considerations in relation to ptosis...
Check the baseline
“It’s always good to establish the baseline appearance with photographic evidence,” she advises. “Discuss pre-existing asymmetry, as well as amend treatment plans if there is ptosis evident pre-treatment.”
Use your medical knowledge
“We’re concentrating on botulinum toxin complications here, but be aware of other causes of ptosis,” counsels Dr Kal. “These may be congenital or acquired (ageing, nerve or muscle issues). It’s useful to acknowledge that baseline ptosis will become more obvious as a patient ages, as well as with certain botulinum toxin treatments.”
Review ptosis patients in person
Dr Kal notes that, “The cause of eyelid and eyebrow ptosis is the key to treatment. In reality, the clinical picture may be elusive and difficult to diagnose. Examination is key to deciding so an in-person evaluation is more effective here. This will help you to understand the concern, as well as manage the journey of the patient’s disappointment with the outcome.”

PREVENTING AND PROVIDING RELIEF FROM UPPER EYELID PTOSIS
“The levator palpebrae muscle usually pulls the eyelid upwards,” states Dr Kal. “If botulinum toxin tracks into this, upper eyelid ptosis is likely.”
“It can be prevented by keeping lateral corrugator injections superficial and pointing away from the orbit when treating the frown area.”
“Additionally, it’s useful to isolate the muscle when treating it. Do this by picking it up and injecting intradermally,” she instructs.
“Clinically, this kind of ptosis is usually unilateral and the iris becomes partially covered by the upper eyelid.” She adds, “It may also be associated with a dry eye.”
“If there is functional deficit, it can be treated with apraclonidine 0.5% topically, if not contraindicated. This is an off-licence indication, providing a temporary 1-3mm lift of the eyelid, via its alpha2-adrenergic agonist action on Muller’s muscle.”

HOW TO IDENTIFY, PREVENT AND CORRECT EYEBROW PTOSIS
“Eyebrow ptosis is a more common concern than upper eyelid ptosis,” observes Dr Kal.
“It’s the descent of the eyebrow as a result of tissue pushing downwards on the eyelid as the frontalis, normally an elevator, drops. With frontalis hyperactivity, patients are constantly using the frontalis to raise their eyebrows for daily visual function. As such, they’re prone to eyebrow ptosis if they have toxin treatment of the forehead.”
She advises, “Eyebrow ptosis can also occur if the dose of toxin placed in the frontalis is too high. Inadvertently injecting too low into the frontalis muscle (eg. with glabella complex treatment which has been placed too high), or catching the frontalis laterally when treating the lateral corrugator, can also cause brow ptosis. Therefore, consider not treating the forehead, lessening the dose or treating high in the frontalis, if there’s pre-existing lid heaviness and frontalis hyperactivity.”
Dr Kal continues, “Patients may present with a functional deficit, for example, having to lift their lid to apply makeup rather than an obvious eyebrow droop. In terms of clinical signs, the iris is more visible, and the brow is immobile. This may improve without treatment.”
“Alternatively, you may opt to treat the residual corrugator, procerus and orbicularis oculi activity to counteract frontalis drop. Some practitioners advocate exercising or stimulating the frontalis muscle as treatment too.”
THE RIGHT MINDSET FOR DEALING WITH POTENTIAL COMPLICATIONS
Harley Academy founder, Dr Tristan Mehta has spoken previously about the importance of overcoming the fear of causing complications. As an aesthetics practitioner you need to be ok with the possibility of causing complications and managing them.
No one wants to cause ptosis, however, you are almost guaranteed to come across this during your practice, especially as you start to treat more patients. It can – and does – happen to injectors of all levels.
What you need to fully grasp and be prepared for is how you’ll manage these situations if they arise. When it comes to managing eyelid and eyebrow ptosis, Dr Kal’s advice is a great starting point which we hope you find useful.
These complications are also covered in the eLearning for our industry-leading Level 7 Diploma in Botox & Dermal Fillers and our Fast Track Level 7. This Ofqual-regulated and JCCP backed, Master’s level qualification is open to licensed doctors, dentists, nurses and midwives.
Personalised information about this, and all our aesthetics training courses, can be obtained by booking a call with our courses team, who’ll be happy to guide you through your best options.
All information correct at the time of publication.
Download our full prospectus
Browse all our injectables, dermal fillers and cosmetic dermatology courses in one document
By submitting this form, you agree to receive marketing about our products, events, promotions and exclusive content. Consent is not a condition of purchase, and no purchase is necessary. Message frequency varies. View our Privacy Policy and Terms & Conditions
Attend our FREE open evening
If you're not sure which course is right for you, let us help
Join us online or in-person at our free open evening to learn more
Our Partners













STAY INFORMED
Sign up to receive industry news, careers advice, special offers and information on Harley Academy courses and services

