Dermal Filler Migration Prevention and Management
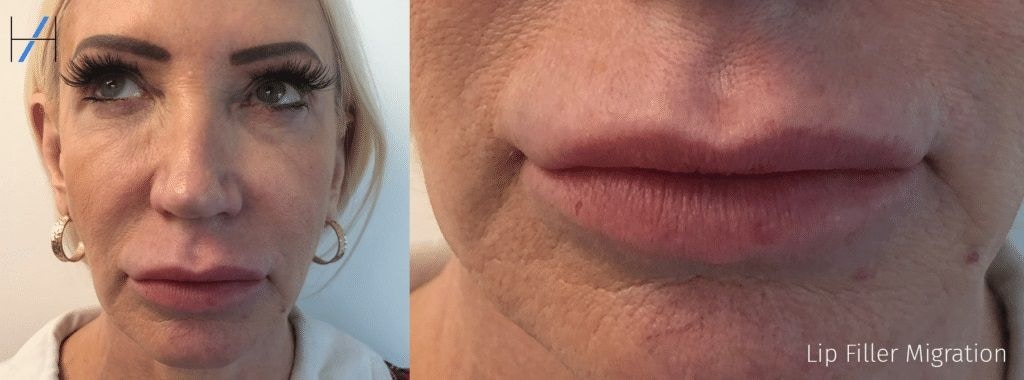
Dermal filler migration is one of the most frequently seen aesthetic medicine complications. As such, it’s vital injectors know how to prevent, identify and manage this effect.
We spoke to Dr Janine Rothburn to find out everything new injectors need to know about filler migration. She is an experienced aesthetic doctor, dental surgeon and clinical trainer at Harley Academy.
Here Dr Janine answers the most common questions about dermal filler migration alongside her own expert advice…
What causes filler migration and how does it present?
“Filler migration is the movement of dermal filler from its intended injection site to another site,” explains Dr Janine.
“There are various reasons as to why it occurs, including poor injection technique, poor product choice for a particular indication, massaging of the area, muscle activity, lymphatic spread, intravascular injection and pressure-induced displacement.”
She further notes that, “Filler migration presents most commonly around the lips and under the eyes.”
How do you prevent filler migration?
“To prevent filler migration, use small volumes of product in a single session, ensuring the chosen product is suitable for that area of the face,” advises Dr Janine.
“Understanding anatomy and the layers of the face to ensure the correct product is used in the correct anatomical area is also fundamental to successful treatment,” she counsels. Noting this will help in “minimising the risk of filler migration”.

How do you treat filler migration?
Dr Janine offers her advice for a couple of different options for treating dermal filler migration:
“The first option is leaving the filler and trying to massage the area and see if the filler will start to break down naturally. However, recent studies using MRI scans have provided evidence that fillers can actually last much longer than we originally thought,” she states.
“The second option is to use hyaluronidase – often referred to by the brand name, Hyalase,” Dr Janine explains, “This is an enzyme that breaks down the hyaluronic acid found in dermal filler. Using it to dissolve dermal filler is actually an off-label use of hyaluronidase. Despite this, it’s considered the gold standard in aesthetic medicine for treating filler migration and other filler complications. The enzyme will break down hyaluronic acid-based dermal fillers.”
How do you diagnose dermal filler migration?
“When diagnosing filler migration, look and feel the area of the face, as well as taking photographs from different angles. Asking your patient about their previous aesthetic history is also paramount. If you are unsure or concerned about any migration present, don’t be afraid to ask a colleague for a second opinion,” advises Dr Janine.
For solo practitioners, reach out to your network – whether this is a WhatsApp group or a professional platform such as Comma – to get the advice you need. Just make sure you have patient consent to do so first if you are posting any specific details or images.
“Aesthetic medicine is a specialty that is progressing,” Dr Janine adds. “Ultrasound devices are also becoming a new means of diagnosing and guiding treatment for filler migration.”
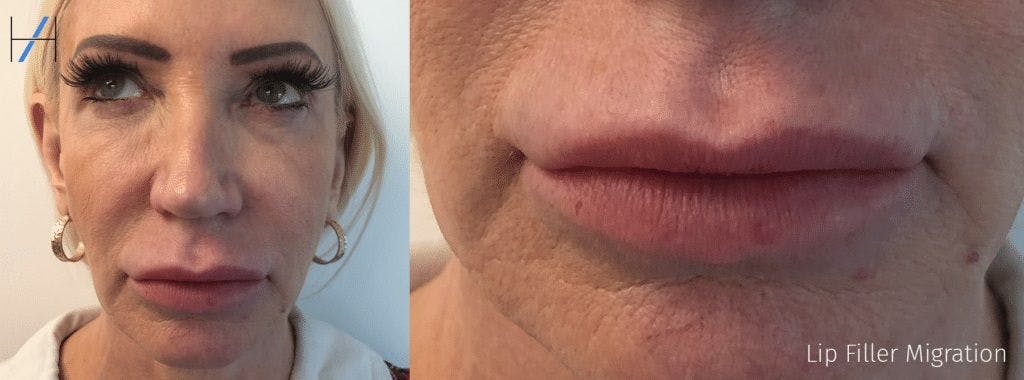
What’s your advice for guiding your patient through this process?
“My advice for guiding a patient through the process of diagnosing and correcting filler migration is communication,” reveals Dr Janine. “Explain the process clearly to the patient and give them the options of leaving and not re-filling, or dissolving the filler. It’s important to make sure they understand the risks and benefits involved with dissolving the filler. Obtaining informed consent is vital in this process. After dissolving the migrated filler, the area can be re-filled again after 14 days.”
Learning more about dermal filler migration
There are three aesthetics training course options for those of you who wish to explore this topic in more depth.
Level 7 Diploma in Botox & Dermal Fillers
Our industry-leading postgraduate injectables training course for licensed doctors, dentists, nurses and midwives. This provides a Master’s level education in aesthetic medicine and is suitable for beginners to intermediate aesthetic practitioners.
Our Level 7 experience can be tailored to your needs, with Fast Track (for more experienced injectors) and Cosmetic Dermatology options also available. However, each Level 7 course covers…
- Facial anatomy and skin ageing.
- Product properties and the fundamentals of botulinum toxin A and dermal fillers.
- Psychology, patient consultation and selection.
- Engaging eLearning which can be completed at your own pace and used as a reference tool throughout your career.
- Practical mentoring sessions treating real patients to build your confidence and hone your injecting techniques.
- Identifying, preventing and treating soft tissue filler complications including migration.
- Professionalism, law and ethics in aesthetic medicine.
- Aesthetics business marketing.
Preventing and Managing Complications
This eLearning course offers a convenient way to enjoy top quality training in dermal filler complications.
Build your knowledge to boost your confidence when it comes to spotting and dealing with potential soft tissue filler complications. In addition to learning the difference between a side effect and a complication, you’ll also cover:
- Relevant anatomy and pathophysiology.
- Exploring complications including anaphylaxis, dermal filler migration, inflammatory nodules, malar oedema, Tyndall effect and vascular occlusion.
- Real life case studies where complications have occurred.
- How to prevent and treat complications, including emergency protocols which are provided as downloads for you to keep and use in your practice.
- Using hyaluronidase in both critical and non-critical scenarios.

Advanced Complications Management Masterclass
In addition to receiving the above eLearning training, this intimate Advanced Masterclass allows you to explore filler complications more fully. You will also learn about Botox complications during this full day session. Breakfast, lunch and refreshments are provided so you can focus on really getting the most from your Masterclass.
Led by an experienced Harley Academy mentor, you will develop an in-depth knowledge of complications prevention, identification and management. This is aided by real life case studies and practical, guided injecting.
- Learn about immediate, early and delayed complications.
- Cover additional complications including brow and lid ptosis and mephisto.
- Mentored mannequin injecting practice.
- Emergency toolkit advice.
- Focus on making you a more confident practitioner.
- Ask questions throughout.

You may also wish to consider 1:1 Injectables Training Sessions
If you have already completed a solid complications prevention and management course but still have areas you’re unsure about, mentoring may work for you.
Our private one-on-one mentoring is not intended to cover complications in great depth. However, this popular form of aesthetic medicine tutoring provides you with a fantastic platform.
Our 1:1 Injectables Training Sessions involve you consulting and treating your own patient, overseen by a specialist mentor. They are designed to help you focus on improving your injecting skills in specific areas.
During these sessions you are welcome to ask your trainer as many questions as you like. So, if you’d like their advice on relevant complications, they’ll be able to help you with this. For example, the 1:1 Training in Perioral and Lip Filler is a great time to explore lip filler migration. Just remember to take notes!
Patient safety is at the core of our business and we want it to be at the heart of yours too. This is why we touch on complications to various extents no matter which training pathway you follow.
If all these options are overwhelming, just get in touch and we’d be happy to talk you through your best options.











