Acne Treatment For Transgender Men
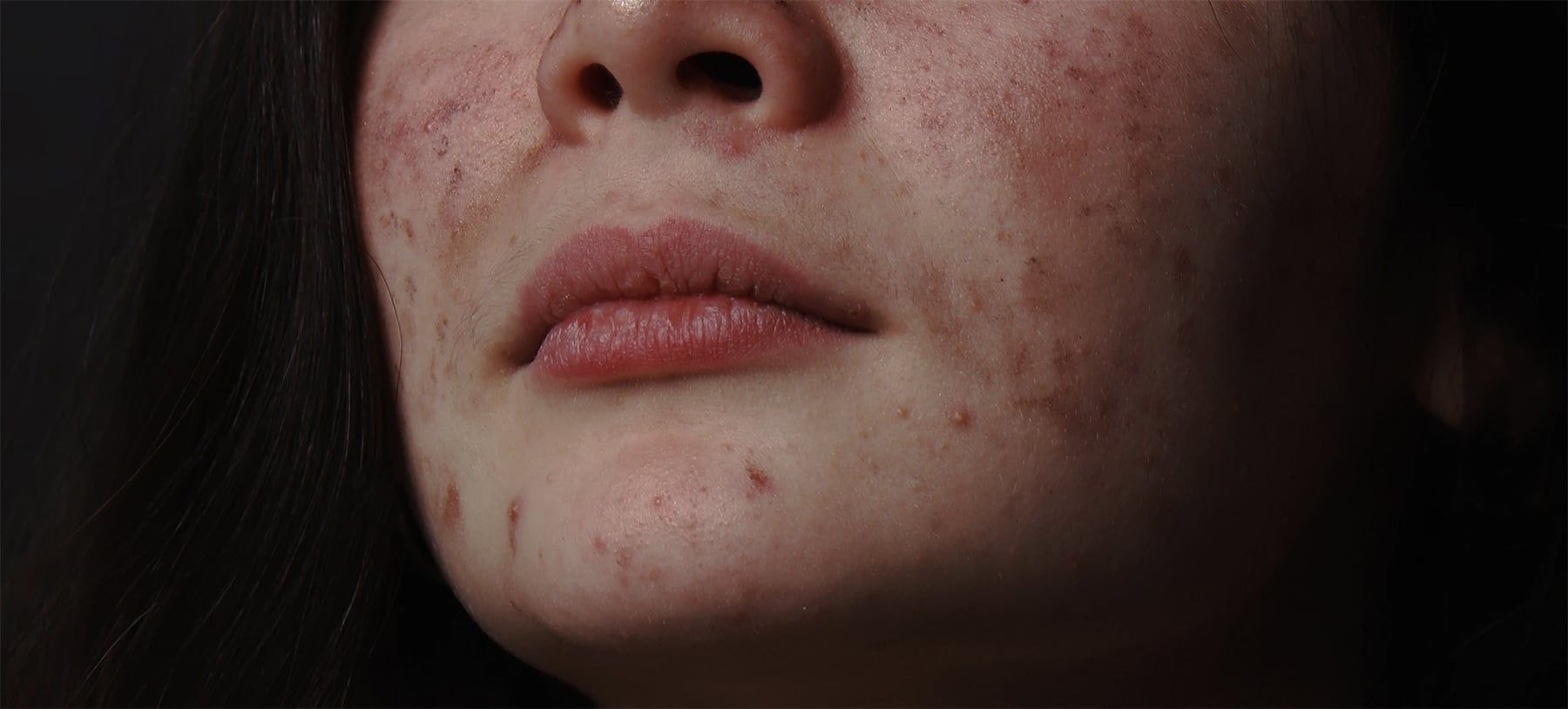
As a recent study outlines why acne is common among female-to-male (FTM) transgender patients receiving hormone therapy, we explore acne treatment for transgender men.
Both acne and being transgender have been separately linked to depression and higher rates of suicide. Therefore, understanding this issue and providing a solution in a welcoming space can be extremely beneficial to trans men.
This is especially true of adolescent patients who are able to start testosterone therapy from 16 years of age.
Masculinising hormone therapy and acne
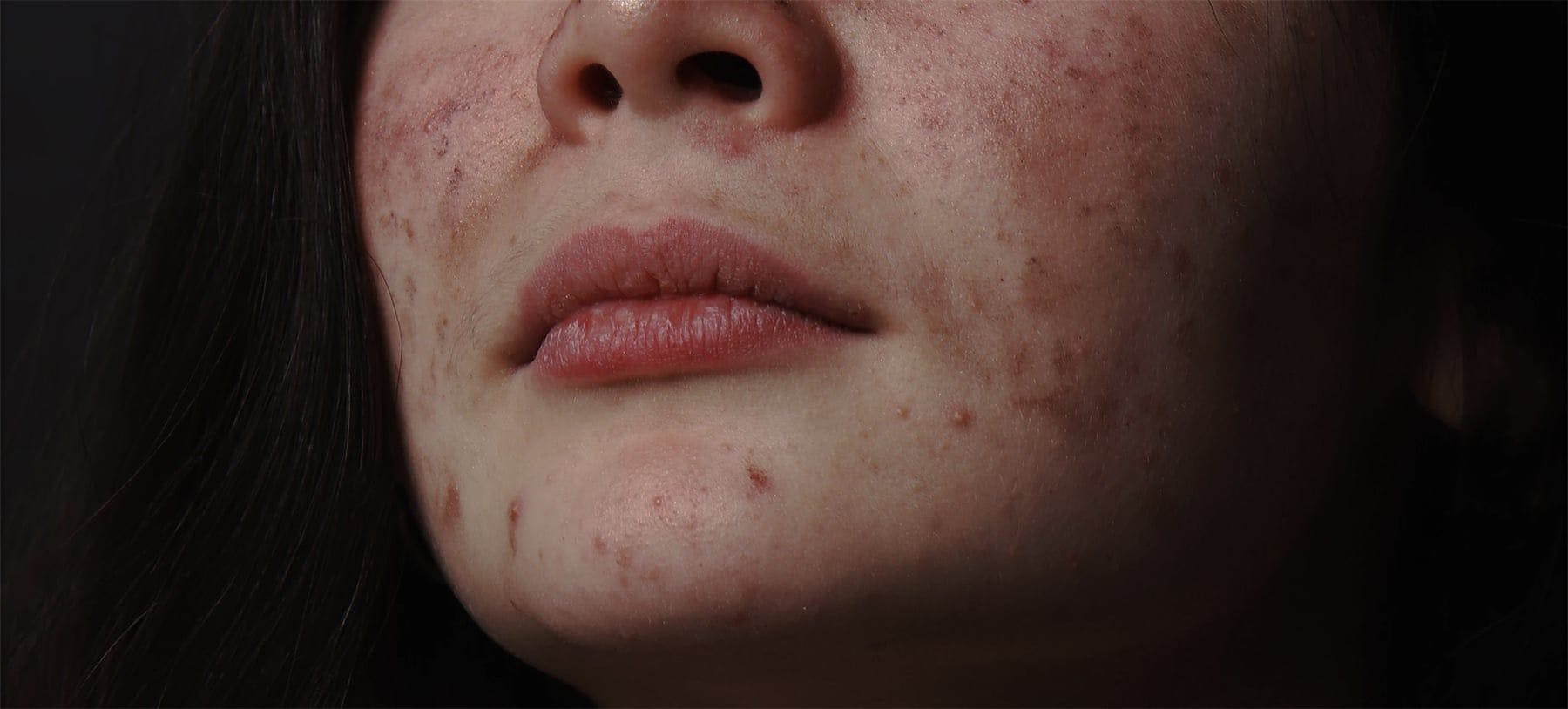
It is already well known that acne often presents in transgender men undergoing masculinising hormone therapy (MHT) involving testosterone. This type of treatment is beneficial for achieving secondary male characteristics such as a deeper voice, hair and body fat patterning, virilisation and suppressing menstruation. However, due to the elevation of androgen levels, increased sebum production may occur and acne is likely.
Acne in transgender men on MHT is generally thought to become visible within the first six months of starting testosterone treatment.
American research published in the JAMA Dermatology journal notes that over a third (31.1 per cent) of its study cohort of 988 FTM patients using MHT experienced acne. It was also most significantly associated with the 18-21 year age group. It is relevant to note that the minimum age requirement for participants was 18 years.
This retrospective study detailed the following findings:
“For 988 patients (median age, 25.8 years; interquartile range, 20.8-28.2 years), there was an overall acne prevalence of 31.1% (n = 307). The 1-year post-MHT acne incidence proportion was 19.0% and the 2-year incidence proportion was 25.1%. A younger age at MHT initiation was associated with a higher likelihood of developing acne, with a median of 22.4 years (interquartile range, 19.7-25.6 years) among patients who developed acne vs 24.7 years (interquartile range, 21.3-29.4 years) among patients who did not (P = .002).”
Treating acne in trans male patients
These study findings certainly point to MHT as a clinical risk factor which should be considered when diagnosing acne in trans male patients. It also shows that acne treatment for transgender men who are undergoing MHT may need additional considerations compared to non-transgender patients.
“Generally, the standard guidelines for the treatment of acne can be followed in treating these patients; however, several medical, social and psychological factors should be considered,” states research from New York, USA, published in the British Journal of Dermatology.
Female to male transgender patients should be treated as male – from both social and medical points of view. For example, a trans man should not be prescribed anti-androgens nor birth control to help manage acne.
You may also consider working with the doctor helping them with their transition as testosterone therapy can often be adjusted. This may reduce the severity of the acne, making it easier to manage.
Although isotretinoin is currently not thought to be linked to depression and has been shown to work well for many trans male patients, it requires oversight where the patient has the potential for mental distress. Furthermore, if the patient is receiving MHT and using isotretinoin, liver function may be adversely affected so regular checks are necessary.
Cosmetic dermatology and injectable solutions for acne and acne scarring

Cosmetic dermatology options for acne treatment can be of great value, especially where a patient is contraindicated for drugs such as isotretinoin.
A course of chemical peels can offer acne relief whilst microneedling is an excellent treatment for acne scarring. Both can also help to improve the patient’s skin texture. As such, these are some of the frontline options to consider when formulating an acne treatment plan for trans male patients.
On the injectables side, soft tissue filler may be used to reduce acne scarring by revolumising these areas. This can provide an almost instant result which patients love to see.
Whichever options you and your patient decide are in their best interest, just remember to conduct a thorough clinical consultation first. Remember to refer patients with moderate to severe acne to a dermatologist who can provide specialist care.
You may wish to allow a longer appointment time than usual to fully explore the medical, psychological and social factors involved, especially if you are inexperienced in treating transgender patients.
Once you and your patient connect and start to see the results of your treatment plan, this should be a hugely rewarding experience for both of you.
Should you find yourself in need of a second opinion, or want to run ideas for how best to approach your patient’s treatment, always ask your professional network. Whether this is a WhatsApp group of your peers or a dedicated medical aesthetics platform such as Comma, you’re bound to find helpful suggestions and reassuring support to ensure you provide optimal treatment.
All information correct at time of publication
Download our full prospectus
Browse all our injectables, dermal fillers and cosmetic dermatology courses in one document
By submitting this form, you agree to receive marketing about our products, events, promotions and exclusive content. Consent is not a condition of purchase, and no purchase is necessary. Message frequency varies. View our Privacy Policy and Terms & Conditions
Attend our FREE open evening
If you're not sure which course is right for you, let us help
Join us online or in-person at our free open evening to learn more
Our Partners















STAY INFORMED
Sign up to receive industry news, careers advice, special offers and information on Harley Academy courses and services

