Visual Loss From Dermal Fillers Case

Vascular occlusion (VO) leading to vision loss from dermal fillers is most aesthetics practitioners’ worst nightmare.
A 2019 case involving a 29 year old woman who lost her sight following non-surgical rhinoplasty was published in the European Journal of Opthamology. Her liquid nose job was performed by a healthcare professional who was not registered with a governing body.
Here we look at this case report and speak to one of its authors – Harley Academy graduate, Dr Rahila Zakir. As well as examining what steps injectors can take to prevent vascular occlusions and ocular complications.

Ptosis, visual loss and ophthalmoplegia
A team from the Western Eye Hospital reported how a 29 year old woman “presented to the eye casualty department with sudden visual loss, ptosis and ophthalmoplegia after having had non-surgical rhinoplasty in a beauty salon in West London”.
Ophthalmoplegia is a paralysis or weakness of the eye muscles.
The patient’s symptoms persisted despite prompt treatment.
“Attempts from the patient and medical services to report the incident (to trading standards and the police) were to no avail,” the research authors note.
They concluded that this case “highlights the poor treatment response to filler-related ophthalmic complications. It is also evident that in the United Kingdom, there appears to be poor regulation in the use of these products, a lack of clear guidelines for the management of their complications and finally no recourse for patients to challenge practitioners who lack medical registration and are not held accountable.”
“This case report illustrates the potentially irreversible consequence of visual loss with nose filler. It is an increasingly popular treatment which can have a profoundly positive impact on self esteem. But it does carry rare, but high impact, risk with life-changing consequences. We need to carefully consider who delivers these advanced treatments and the impact on the NHS, acutely and in the longer term,” advises Dr Kalpna Pindolia, director of education at Harley Academy.
“This is the UK – everything is tightly regulated for our protection yet non-medical injectors are still allowed to practice.” DR RAHILA ZAKIR, CONSULTANT OPHTHALMOLOGIST, VITREORETINAL SURGEON & LEVEL 7 GRADUATE
Devastating gaps in the UK system
One of the study’s authors, Dr Rahila Zakir, is a Harley Academy Level 7 Diploma in Botox and Dermal Fillers graduate. We spoke to her about how she felt, dealing with this interesting yet tragic case.
“It was devastating that there was nothing we could do for her. Usually with ophthalmic complications from dermal filler some sight is retained, whether it’s blurry or partial, but there was nothing we could do and that was hard,” explained Dr Zakir. “The patient was also embarrassed at this happening as a result of a cosmetic procedure, which was tough to see.”
“There was anger at the lack of recourse. There was no one for her to turn to and nothing that could be done. She has to suffer these lifelong consequences due to falling through gaps in the system, which is really frustrating to witness.
“This is the UK – everything is tightly regulated for our protection yet non-medical injectors are still allowed to practice.
“I’m a surgeon. I understand that complications happen even in the best hands. It’s about being trained to identify and minimise risk, as well as having a good team around you so that, should any adverse events occur, the patient has the proper care straight away and the problem can be managed effectively, allowing for the best possible outcome.”
Can you eliminate the risk of vascular occlusion?
Example of a vascular occlusion following filler administered via needle to treat the nasolabial folds
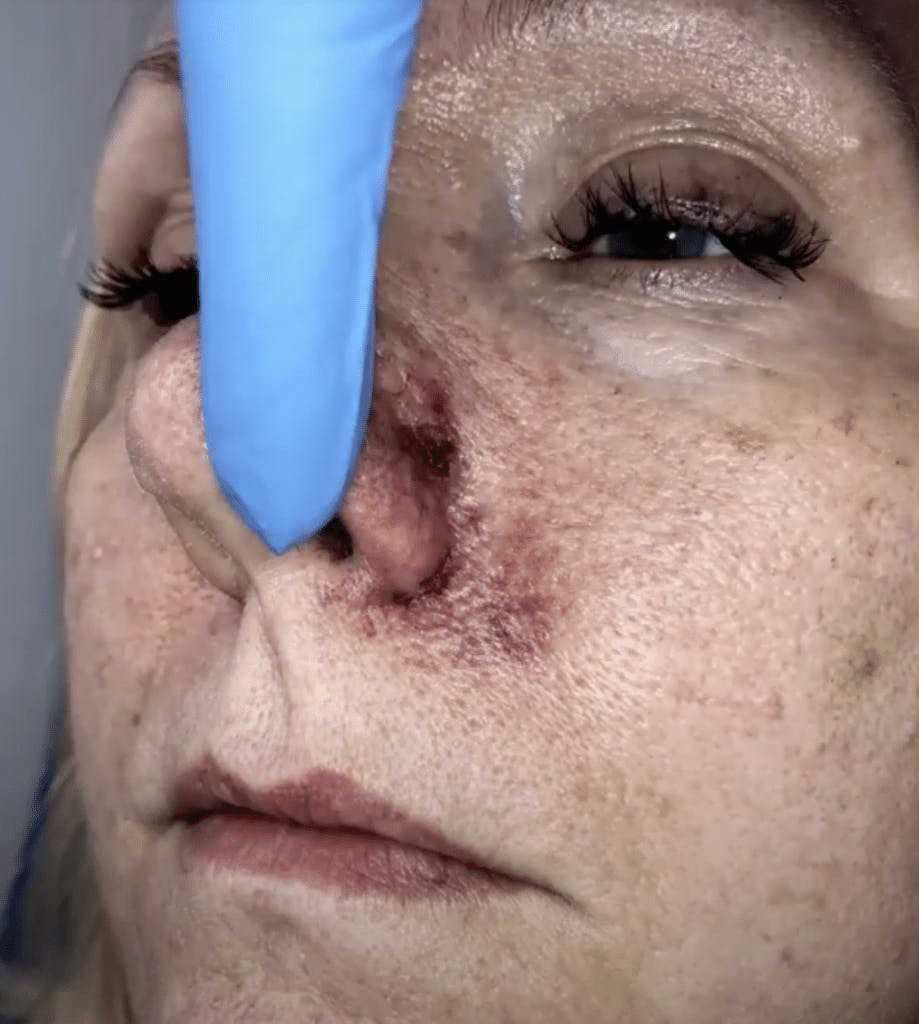
Healthcare professionals are trained to do everything they can to minimise the risk of vascular occlusions and filler blindness.
This requires a solid knowledge of facial anatomy, a good, steady injecting technique and having a well-rehearsed emergency protocol.
As we know, there are many non-medical injectors who are untrained and do not have the necessary anatomical or practical knowledge for this. However, it is worth noting that a VO can happen to even the most experienced injector.
Whilst using a cannula is considered to reduce the risk of vascular occlusion, it may still occur, as this case study shows. However, complications such as VO are more likely when injecting trickier areas such as the nose or lips.
All information correct at the time of publication.
Download our full prospectus
Browse all our injectables, dermal fillers and cosmetic dermatology courses in one document
By submitting this form, you agree to receive marketing about our products, events, promotions and exclusive content. Consent is not a condition of purchase, and no purchase is necessary. Message frequency varies. View our Privacy Policy and Terms & Conditions
Attend our FREE open evening
If you're not sure which course is right for you, let us help
Join us online or in-person at our free open evening to learn more
Our Partners















STAY INFORMED
Sign up to receive industry news, careers advice, special offers and information on Harley Academy courses and services

