Vascular Occlusion Advice For Aesthetics Practitioners
Vascular occlusions - now more accurately referred to as vascular 'events' - can be a huge concern as a new aesthetics practitioner.
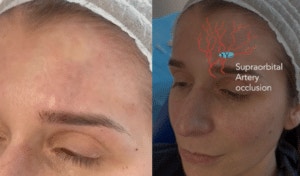
Harley Academy students and medical aesthetics professionals may have seen a rare complication on Comma. A video case study of a supraorbital artery vascular occlusion was posted to the specialist networking platform.
Causing a vascular occlusion (VO) is likely to happen to every injector at some point, so we wanted to provide some further information on this story.
Read on for expert advice on how to prevent, identify and manage a vascular occlusion.
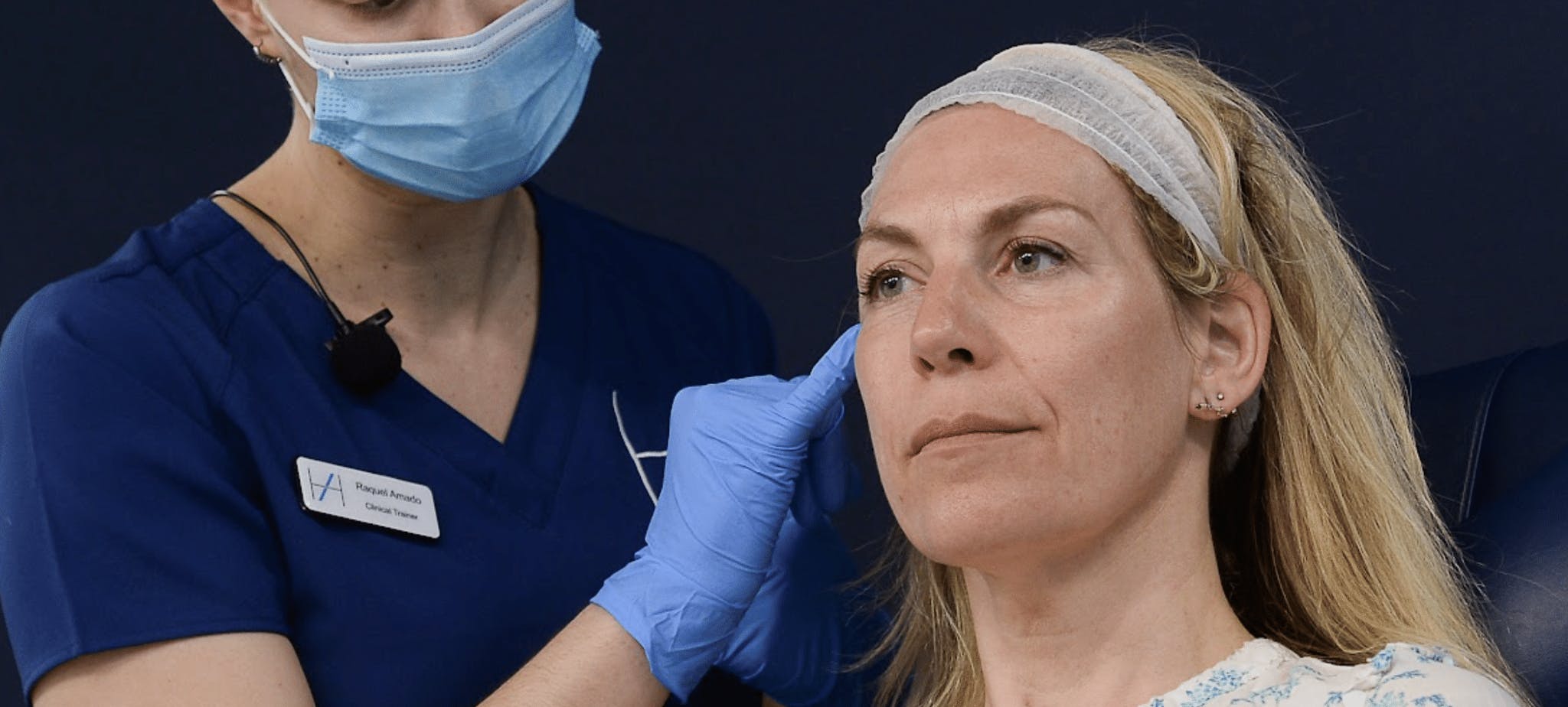
Vascular occlusion advice for new aesthetic practitioners
Dr Raquel Amado is an aesthetic medicine expert who specialises in taking an holistic approach to facial enhancements at her own practice. She was also a senior clinical trainer at Harley Academy at the time of publication.
We spoke to her about supraorbital artery vascular occlusion, how to prevent vascular events and the signs to look for if a VO is suspected…
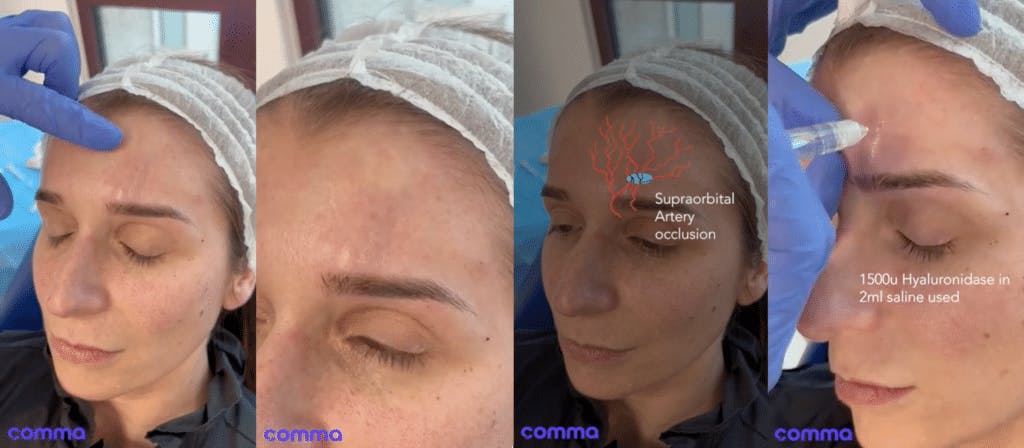
What causes a supraorbital artery vascular occlusion?
A vascular occlusion happens when dermal filler blocks a blood vessel. It may be a complete occlusion or partial occlusion, resulting in a diminished blood supply of the corresponding angiosome. Emboli can also travel further up the vascular tree from the occluded area. If left untreated, vascular occlusions can result in necrosis of the tissue.
The case that was shared on the Comma network involves the supraorbital artery. This is a branch of the ophthalmic artery and, therefore, there is a communication route of blood flow between the internal and external carotid system. This means this complication has the potential to cause blindness – often referred to as “filler blindness”.
The supraorbital artery emerges on the face through the supraorbital notch or foramen to irrigate the forehead.
The deep branch of the supraorbital artery changes plane from deep to superficial to the frontalis muscle on average between 13-14 mm from the superior orbital rim.*
Although the patient in this Comma case was injected in the supraperiosteal plane, within “safe” parameters for the region, an occlusion occurred. This just goes to show that there isn’t a safe area to inject in and anatomy is very variable.
How do you prevent vascular events from happening?
In order to prevent vascular occlusions, the most important factor is understanding the depth of injection.
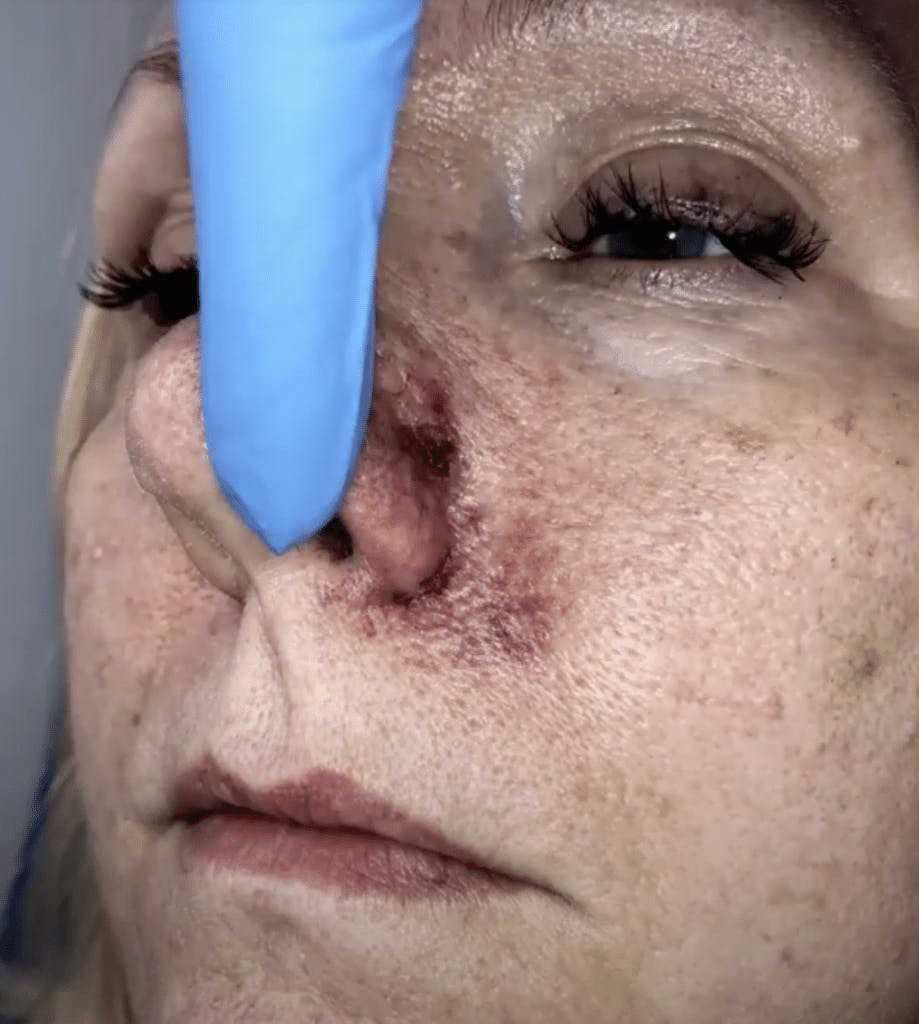
Below is an example of a vascular occlusion post-nasolabial fold filler
Everyone’s anatomy is different and distribution is extremely variable, however, depth is a more reliable parameter.
Therefore, it’s crucial you have an in-depth knowledge of which layer the arteries are more likely to be in and also if there are any anastomoses.
This is relevant as, in the case of an occlusion, your patient may complain of referred pain or you could see some blanching further from the injection site.
Always look at the surrounding skin, not just the area you injected.
Dr Raquel’s 6 top tips for preventing vascular occlusion:
1. Inject small amounts, slowly with low pressure
2. Use the appropriate product in the right layer.
3. Whenever possible, use a cannula instead of a needle.
4. Fully understand anatomy, especially depth of injection.
5. Get adequate aesthetic medicine training and keep updating your knowledge.
6. Ensure you can identify higher risk patients – those that have had trauma, surgery or a possible change in anatomy are at higher risk.
How can you spot a vascular occlusion?
Below is an example of a vascular event following lip filler
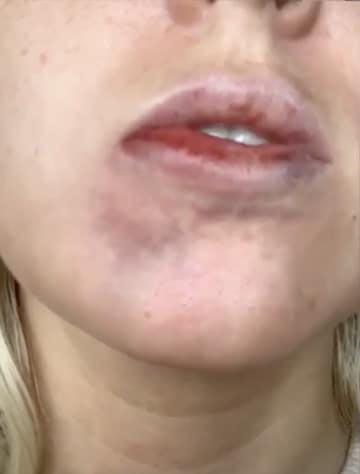
After injecting, there are a number of signs to look out for which may signify a vascular event. These include:
– Blanching.
– Mottling of the skin – this was not observed in this case because it was detected straight after injection and dissolved before this occurred.
– Slow capillary refill of more than 3 seconds.
– Sometimes pain. This did not occur in this case as the patient just felt increased pressure in the area.
In this case specifically, we saw swelling – increased pressure in the supraorbital artery and the blanching was pretty instant.
How do you manage a vascular occlusion?
Managing a vascular occlusion can be broken down into the following steps…
– Keep calm!
– Always have enough hyaluronidase at hand, as well as other emergency drugs such as adrenaline. Make sure these medications are in date.
– Ensure you have your emergency protocols to hand.
– Ideally you should have a referring protocol in place in case help is needed.
– Reassure and follow up with your patient.
As part of our industry-leading injectables qualification, the Level 7 Diploma in Botox and Dermal Fillers, we provide access to our Preventing and Managing Filler Complications online course.
This dedicated short eLearning course on preventing complications is also available to aesthetic practitioners who are healthcare professionals. You don't have to be a Harley Academy Level 7 trainee - you can, in fact, purchase this valuable educational tool online.
For further details on medical aesthetics training for both beginners and more experienced aesthetic practitioners, book a call with our course advisors.
All information correct at the time of publication
* Reference article :Sebastian Cotofana, MD, PhD, Peter J Velthuis, MD, PhD, Michael Alfertshofer, Konstantin Frank, MD, Vince Bertucci, MD, Kate Beleznay, MD, Arthur Swift, MD, Diana L Gavril, MD, Nirusha Lachman, PhD, Leonie Schelke, MD, The Change of Plane of the Supratrochlear and Supraorbital Arteries in the Forehead—An Ultrasound-Based Investigation, Aesthetic Surgery Journal, Volume 41, Issue 11, November 2021, Pages NP1589–NP1598,
Download our full prospectus
Browse all our injectables, dermal fillers and cosmetic dermatology courses in one document
By submitting this form, you agree to receive marketing about our products, events, promotions and exclusive content. Consent is not a condition of purchase, and no purchase is necessary. Message frequency varies. View our Privacy Policy and Terms & Conditions
Attend our FREE open evening
If you're not sure which course is right for you, let us help
Join us online or in-person at our free open evening to learn more
Our Partners















STAY INFORMED
Sign up to receive industry news, careers advice, special offers and information on Harley Academy courses and services

