Patient Communication: How To Deal With Difficult Patients

There will be challenging patients in any service-based environment. As aesthetic practitioners, perhaps we are more susceptible to challenging encounters because we meet a diverse range of people with an agenda of desiring physical change on the basis of deep-seated psychological drivers.
Challenging situations can escalate, leading to the patient to believe they have been mistreated or harmed. This view can be expressed as anxiety, fear, anger or distress.
This article explains some important methods of patient communication you can use for dealing with difficult patients.
Prevention is better than cure
From the start, the consultation process is a valuable opportunity to establish rapport. This collaborative process of establishing concerns and expectations empowers both patient and practitioner. As the expert, you can:
– Educate your patient
– Discuss safety
– Explore the meaning of realistic expectations.
Alignment of agendas between parties allows for management of risk and realistic recognition of likely outcomes. Understanding the true value of using lower risk procedures to achieve desired outcomes reduces the likelihood of complaints. Under-promising and over-delivering results is also a tried and tested recipe for patient satisfaction.
Understanding the complex goals, expectations, and psychological needs of patients seeking aesthetic treatments are central aspects of patient care and achieving patient satisfaction, hence avoiding dissatisfaction.
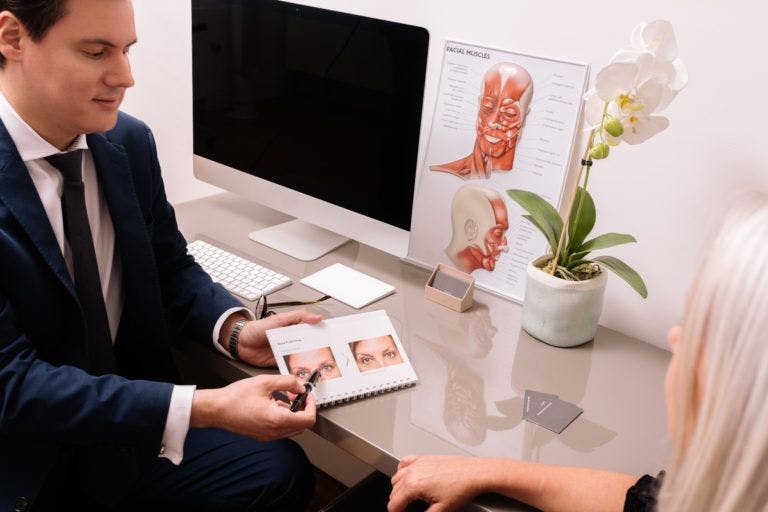
Red Flags
The identification of red flags and use of your gut instinct are powerful predictors of potential concern later. The following features may suggest that there is a higher risk of problems later:
– Previous multiple poor experiences by the patient (especially previous litigation) For instance, has the patient had several treatments by various practitioners with unsuccessful outcomes?
– Practitioner hoppers and hagglers Does the patient see lots of practitioners and/or strongly barter for discounted treatment?
– Body dysmorphic disorder (BDD) Does the patient express severe anxiety about a perceived flaw that, firstly you cannot see, and secondly, significantly affects their day-to-day experiences, for instance at social functions or work?
– Unrealistic expectations For example, does the patient expect major change with little product?
– The VIP Are they a celebrity in the public eye, or a lawyer in court, with high pressure on them concerning their physical appearance?
– Treatments preceding major events Have you got a bridezilla in your consulting room?
– Multiple calls or overly anxious behaviour Have the number of interactions preceding treatment been excessive or is the patient unreasonably nervous?

The ‘do not treat’ option
Both patient selection and deselection are crucial. Remember there is always the option of ‘do not treat’ at the outset rather than firefighting later. Using colleagues as a resource, seeking second opinions, can also be a useful form of support, although ultimately the path you decide to take will be yours to contend with.
Why are challenging patients important to engage with?
Unsatisfied patients can defame the practitioner, file complaints and may even initiate litigation. Promptly addressing patient complaints can decrease this tendency. It is less stressful and time consuming to placate patients who have become challenging in behaviour at the earliest encounter.
4 steps to managing the problem
1. Deal with the specifics
Early intervention is key. Unhurried, calm and private interactions are preferable so as not to add fuel to the fire. Ask the patient what they believe could resolve the issue and decide if that is reasonable, without judgement.
Avoid ‘maybes’ and instead explain firm reasonable choices to restore patient confidence and give back the reins of control, which could mean considering adjustments in treatment. Remember to use your pre-treatment and post-treatment photos to illustrate any points required. Documentation is also crucial, and helps ensure you don’t put yourself in danger.
Remember, apologies do not need to be an acceptance of responsibility. They can be offered for the patient’s unmet expectations and the emotions they are experiencing without indicating culpability.
2. Be empathetic
Belief in the reality of the patient’s expressed concerns and legitimacy of their personal emotions is central. Their feelings are real, whether you believe they are justified or not. Their need for validation is strong, even if it is inappropriate from your perspective. The use of empathy can lead to genuine rapport establishment in complaint resolution.
3. Use good communication skills
Reasonable eye contact A series of reasonable glances instead of intense long stares is more appropriate in these emotional situations
Appropriate and open body language Keep an eye on your posture, and employ gestures and affirmative movements, like head nodding, to express empathy
Proactive listening helps develop solutions By listening attentively, avoiding interruption, and clarifying their statements, you can resonate a caring attitude towards the patient
Employ the power of silence Respectful silence can to allow room for listening and also empowers the patient to feel that they are being heard.
Repeat their concerns back in understandable terms For example, avoid the use of medical jargon and tailor your words to improve understanding between the two parties.

4. Acknowledge and manage your own emotional baggage
Many aesthetic practitioners are not comfortable working with unhappy patients and may experience anxiety when required to do so, particularly in the early days of being in their speciality. The need to defend ourselves is instinctive. However, acceptance and insight of your own emotions is also central with managing these patients well and more comfortably.
After the storm
– Thank the patient and follow up.
– Monitor and follow up your response
– Evaluate and reflect on the situation to prevent recurrence.
Opportunities from challenges
Patient dissatisfaction may still occur, despite meticulous efforts. Maybe, culturally, we could benefit from a perspective shift toward seeing our more-vocal patients as actively engaged in their treatment, rather than challenging in behaviour. There is a lot to learn from such encounters.
And remember amongst the fog of emotions experienced in these challenging situations, there is a person just asking you to ‘help me’. In the end, all patients make us happy right? Some when they arrive, and the occasional one, when they leave…
About the author:
An experienced aesthetics practitioner, assessor and and GMC appraiser, Dr Kalpna Pindolia is Director of Education and Lead Trainer at Harley Academy. This treasured member of our clinical faculty has also run her own successful private practice and now works as an injector at STORY Marylebone. Her holistic approach to treatment, combined with an infectious sense of humour, make her popular with both our patient and student communities alike.
Article last fact-checked: 11 January 2023
Download our full prospectus
Browse all our injectables, dermal fillers and cosmetic dermatology courses in one document
By submitting this form, you agree to receive marketing about our products, events, promotions and exclusive content. Consent is not a condition of purchase, and no purchase is necessary. Message frequency varies. View our Privacy Policy and Terms & Conditions
Attend our FREE open evening
If you're not sure which course is right for you, let us help
Join us online or in-person at our free open evening to learn more
Our Partners















STAY INFORMED
Sign up to receive industry news, careers advice, special offers and information on Harley Academy courses and services

