Managing Facial Overfilled Syndrome in Aesthetics Patients
New research exploring Facial Overfilled Syndrome has some key takeaways for aesthetic practitioners.
Published in the Clinical, Cosmetic & Investigational Dermatology journal, this study considers the rise in ‘excessive or inappropriate use of dermal fillers’.
As we know, many patients fear fillers because of the much publicised “pillow face” effect. This research helps understand how this can happen
In this article we:
- Explain what Facial Overfilled Syndrome is
- Review the findings of this new FOS study
- Explore the signs aesthetic practitioners need to look out for
- Share how to diagnose and manage patients with ‘too much’ and/or displaced filler
- Set out how to decide if you should treat overfilled filler patients.

What is Facial Overfilled Syndrome?
In the aforementioned study, released online in March 2026, Facial Overfilled Syndrome (FOS) is described as being ‘an increasingly prevalent iatrogenic complication resulting from the excessive or inappropriate use of dermal fillers.’
It was further explained to be an ‘adverse event following minimally invasive soft tissue filler injections, typically resulting from excessive use of hyaluronic acid or non-hyaluronic acid fillers in the face, leading to an overly inflated or swollen appearance, and may also cause changes in facial expressions and unnatural volume distribution in the midface’.
The team notes this is clinically significant for ‘causing facial distortion and unnatural dynamics’ which are ‘frequently compounded by profound psychological distress and aesthetic perception biases’.
Why aesthetic practitioners need to understand FOS
As an aesthetic practitioner, you need to develop a deep understanding of where volume naturally lives in a youthful face. This is a vital skill from both a client education and practitioner responsibility perspective.
It’s a foundational practice that separates genuinely skilled clinicians from those who are simply placing product. Without having this type of anatomical and aesthetic literacy, it’s almost impossible to make sound decisions about where to treat, which modality to employ, how much product to use, and crucially, when not to treat.
Understanding product rheology, including how long soft tissue filler can take to truly break down, is also important to get to grips with. Always ask your patients about all previous filler treatments and learn to spot the signs of lingering product.
As patients who’ve been overfilled or have years of filler build-up actively request correction, it’s also important to understand how to manage these cases. Once you know what’s involved, you can make an informed decision as to whether this is appropriate for your level of expertise, or whether you’re better off referring to a more experienced colleague.
What did this research show?
For this project, the Chinese team conducted a comprehensive literature review. This involved relevant original studies, clinical trial data, meta-analyses, and reviews published before November 2025.
The researchers found the ‘pathogenesis of FOS extends beyond mere volumetric excess, driven by a complex triad’. This comprised:
- Anatomical mismatch
- Biomechanical dysregulation
- Cumulative payload of repeated treatments.
‘Clinical hallmarks include resting distortion and unnatural facial animation,’ they advised.
The full research paper sets out additional findings which inform how to spot overfilling, as well as how to manage this specific presentation.
Should you treat aesthetic patients who have an overfilled face?
The question of how to treat patients with Facial Overfilled Syndrome is actually skipping too far ahead. First, you need to ask, “Should I be treating this patient who shows signs of being overfilled?”
By ‘treating’, we mean identifying the issues, dissolving filler and potentially re-treating, whether with fillers or other modalities.
- Are you comfortable that the patient is fit for treatment?
- Do you have the necessary skills and equipment to perform any necessary imaging checks and understand what this data shows you?
- Are you sufficiently experienced and confident in your ability to dissolve filler using hyaluronidase and manage any potential compliations?
If you aren’t checking all of these boxes, you may be better off referring the case to a more experienced colleague, rather than treating yourself. This is a complex area and you must be confident that you’re treating within your competency so, if in doubt, refer.
Red flags that signal Facial Overfilled Syndrome
Before we get into the steps for how to spot these cases, here’s a quick overview of some key diagnostic red flags. The following should always trigger a formal FOS workup:
- History of multiple filler sessions, particularly across several aesthetic practitioners
- Cumulative HA volume exceeding anatomical norms for the region
- Patient-reported or clinician-observed "unnatural" appearance, especially upon animation
- "Setting sun" eyes, midface heaviness, or loss of the ogee curve
- Restricted smile or facial animation
- Palpable nodules or surface irregularities
- Request for additional volume in a patient who is already over-volumised.
7 Steps for how to diagnose FOS
1. Understanding what you're looking for
Before any diagnostic workup, it’s critical to understand what FOS actually represents and looks like.
Given its layered complexity, which we’ve outlined above, your diagnostic approach must assess dynamic facial behaviour, filler type and layer, cumulative treatment history, and the patient's psychological state. Don’t rely solely on assessing their static volume.
2. History-taking during a full clinical consultation
As always, a thorough and structured patient history is non-negotiable. Key areas to explore include:
- Treatment history
- Aesthetic practitioner context
- Patient motivation
- Symptom onset
When asking about their treatment history, you’ll need to establish the full chronology of fillers, including:
- Which products were used (HA vs. non-HA: PLLA, PCL, collagen, permanent fillers)
- Volumes injected per session
- Injection depth (the patient is unlikely to know this so you’ll need to assess and/or contact their practitioner for details)
- Number of sessions
- Time intervals between previous filler treatments.
Find out where they received their treatments before coming to you and who treated them. This can be helpful as some unregulated institutions or injectors may recommend excessive filler use in a single session. They may also use products that are not approved for UK use.
Explore your patient’s aesthetic goals that drove them to seek treatment initially, as well as why they’ve come to you now. The research notes that patients with a history of pursuing homogenised social media-driven aesthetics are at elevated diagnostic risk.
Ask your patient when they first noticed their appearance change, and whether it has worsened progressively. FOS often develops cumulatively across multiple sessions rather than presenting acutely.
It can be helpful for you to ask the patient to show you a photo or video of themselves just before they had filler. This can inform your perception of their baseline.
3. Performing a static facial assessment
Start by assessing your patient’s face with a systematic inspection at rest. Key signs to assess, include:
Midface (highest-risk zone): Look for excess volume in the malar and submalar regions. FOS symptoms to watch out for can include:
- Heavy mid-to-lower face
- "Setting sun" eyes
- Broadened nose
- Round and over-protruding forehead
- Pointy chin.
Periorbital region: The "setting sun" eye symptom is a classic and diagnostically significant marker. This is where downward displacement of the cheek tissues creates a heavy, drooping appearance beneath the eyes.
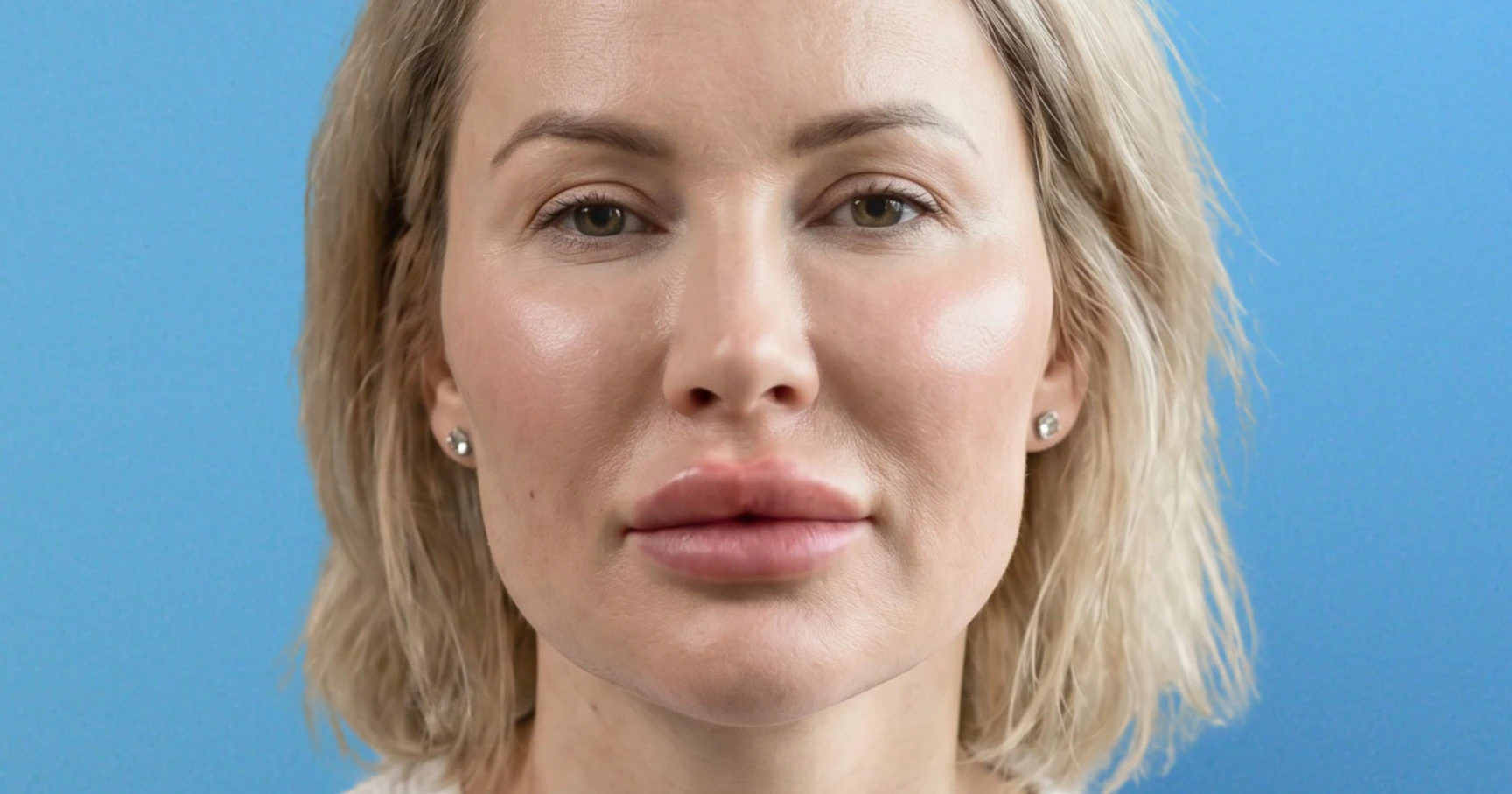
Global facial morphology: Assess whether your patient’s overall proportions would generally be considered to be proportionate. Overfilling the cheeks may cause the midface to protrude excessively. This can make other areas, such as the chin or forehead, appear relatively recessed, causing a disproportionate appearance.
In FOS, you’re typically seeing the triangular ogee curve replaced by a flattened, laterally expanded silhouette. This is often referred to colloquially as "pillow face."
Tissue texture and surface: Always palpate for nodules, irregularities, and areas of abnormal firmness. When excessive filler is injected or unevenly distributed, it may accumulate locally under the skin, leading to uneven surfaces and a stiff texture. These nodules not only compromise aesthetic appearance but may also cause pain or discomfort, especially upon animation.
Skin quality: Does your patient’s skin appear stretched or overly smooth? Look out for the "bread bun" or "mantou" morphology which is characterised by a featureless, convex facial surface that lacks the natural shadows and highlights of three-dimensional facial structure.
4. Dynamic assessment
This is the step most aesthetic practitioners skip and where FOS diagnosis is most commonly under-recognised. Static photographs and resting assessment alone are insufficient.
In most cases, FOS presents as excess midfacial volume and/or as an unnatural smile, which is difficult to detect due to the absence of standardised evaluation methods.
Assess your patient through the full range of facial animation:
- Smiling (both natural and exaggerated): Look for restriction of the oral commissure elevation, bunching of filler material in the cheeks, and an unnatural "frozen" or "stiff" quality to the smile
- Chewing and speaking: Dynamic loading reveals how filler material displaces and whether it restricts muscular mobility
- Raising eyebrows and squinting: Assess for restriction in the upper face if forehead or temporal filler is present
- Profile assessment in animation: Observe the nasolabial fold depth during smiling. Excessive filler in the cheeks often obliterates the nasolabial fold anatomy entirely, which is a big diagnostic red flag!
Facial distortion due to overfilling can be exaggerated by facial expressions and movements. It can worsen with tissue ptosis due to ageing, which means older patients or those with early tissue laxity may present with a more severe dynamic than their resting appearance suggests.
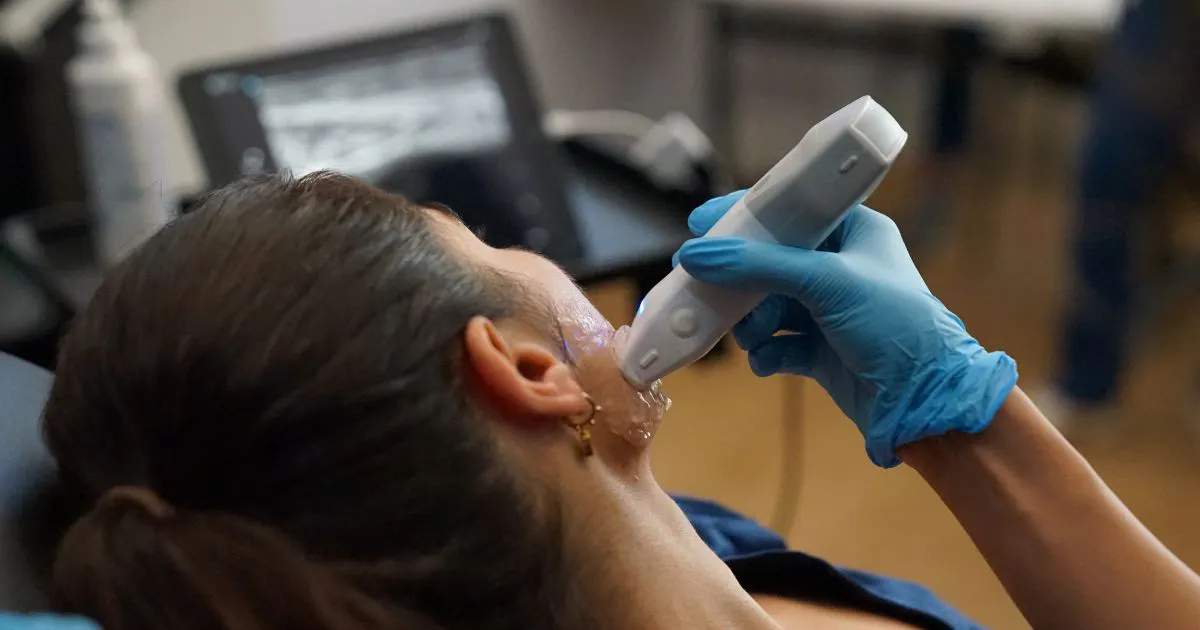
5. Imaging for objective confirmation
Sometimes visual assessment and palpation is just not enough. Ultrasound imaging is becoming more commonplace in aesthetics clinics and plays an essential role in confirming diagnosis. It can also characterise filler distribution, and aid treatment planning.
High-resolution imaging can help you to diagnose FOS by examining the fluid in the superficial tissues of the face. However, it is only useful if you are skilled in these devices and know how to interpret the data they present.
Precisely locating subcutaneous filler distribution, enables you to avoid “injecting blind” and should enhance the accuracy of your corrective interventions. But only if you’re confident that you can accurately read and understand what the ultrasound screen is showing you.
On ultrasound, hyaluronic acid-based fillers appear as hypoechoic (dark) deposits. These can migrate from the layers in which they were originally placed. As such, imaging requires global exploration and layer-specific identification for effective treatment planning.
If you’re not confident in your ability to decipher ultrasound readings correctly, you’re best to refer. Additionally, CT and MRI may be warranted in complex cases with suspected permanent filler, granuloma formation, or vascular compromise.
6. Identifying your patient’s previous filler types
Accurate treatment planning requires understanding what type of filler is present. Start by asking your patient but, be warned, they don’t often have this information. You may wish to ask for their injector’s details, so you can try to obtain this directly from them.
As a general rule:
- Hyaluronic acid-based fillers are soft, compressible on palpation, and reversible
- PLLA and PCL stimulate biocollagen and are not directly reversible
- Permanent fillers (silicone, PMMA) require surgical management.
7. Assessing psychological considerations
There is often a psychological dimension to Facial Overfilled Syndrome. You must formally assess for this during consultation, as it impacts both your diagnosis and management planning.
Explore topics such as:
- What drove your patient to seek filler initially? What outcomes were they hoping for?
- How did they feel about themselves and their appearance before and after these treatments?
- What made them seek help for overfilling and how do they feel about themselves and their appearance now?
- Has their appearance impacted their lifestyle, such as going out less, or their mental health?
This new research clearly states that FOS is frequently compounded by profound psychological distress and aesthetic perception biases. Some of these patients may present requesting more filler rather than correction. As such, screening for body dysmorphic disorder (BDD) is strongly advisable in overfilled cases.
We hope you’ve found this information helpful. For more aesthetic medicine research, explore the Harley Academy Aesthetics Learning System at harleyacademy.ai
All information correct at time of publication
Download our full prospectus
Browse all our injectables, dermal fillers and cosmetic dermatology courses in one document
By submitting this form, you agree to receive marketing about our products, events, promotions and exclusive content. Consent is not a condition of purchase, and no purchase is necessary. Message frequency varies. View our Privacy Policy and Terms & Conditions
Attend our FREE open evening
If you're not sure which course is right for you, let us help
Join us online or in-person at our free open evening to learn more
Our Partners















STAY INFORMED
Sign up to receive industry news, careers advice, special offers and information on Harley Academy courses and services