Lip Filler Vascular Occlusion Case Study
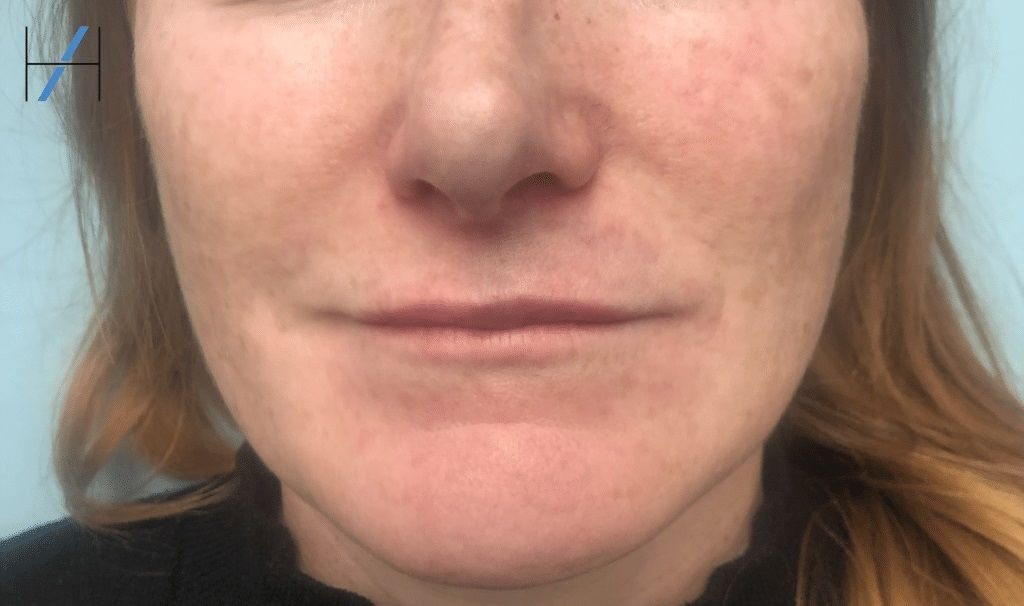
Here we present a lip filler vascular occlusion (VO) study, which was treated by Harley Academy Medical Director, Dr Emily Mehta.
Watch the capillary refill video below then answer the questions about spotting and managing this complication. Then, scroll down to after the VO video to find out how Dr Emily treated this patient.
Lip filler vascular occlusion video
The following patient has just had lip filler which was administered by a healthcare professional using a cannula. This video shows her capillary refill test.
Answer the following questions:
1. Name two signs of vascular occlusion that can occur immediately after occlusion.
2. What does the capillary refill test indicate?
3. What do you believe may have caused this VO?
4. Having identified the VO, how would you treat this patient?
5. The patient also experienced blanching and duskiness at the tip of the nose (as per the image below). Anatomically, what could have caused this?
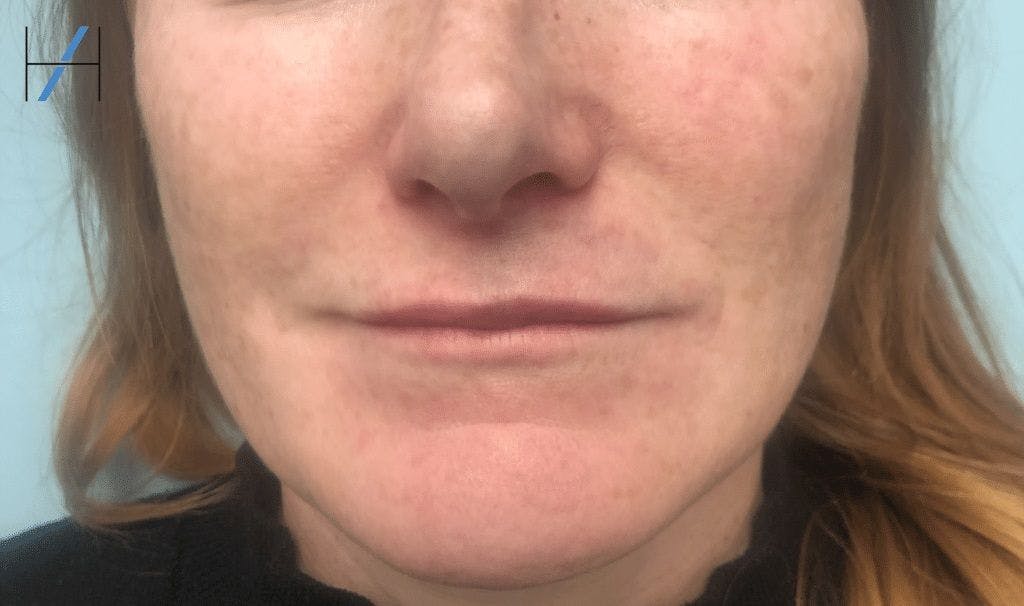
Now, scroll down to find out the answers…
Quiz answers
A) Name three signs or symptoms of vascular occlusion that can occur immediately after occlusion.
Immediately after an occlusion has occurred you may see the following signs:
1. Blanched/Dusky skin discolouration.
2. A slow capillary refill.
3. Pain.
Signs that can occur later (after hours) include blisters, erythema, blue/purple skin discoloration and necrotic tissue breakdown.
B) What does the capillary refill test indicate?
As we’re sure you all know, a capillary refill test allows us to assess how quickly blood is moving through the tissues. The slow capillary refill (longer than 2 seconds) seen in this video indicates that the blood is unable to move freely here. Therefore, this suggests the presence of a local arterial vascular occlusion. This is especially likely when seen alongside the lip filler patient’s other signs such as localised blanching.
C) What do you believe may have caused this VO?
It is generally considered safer to perform filler treatments with a cannula as this can help to minimise the risk of vascular occlusion. In this instance, a 25 gauge (G) cannula was used. However, even in experienced hands, VOs can happen.
Although the precise cause of the lip filler vascular occlusion has not been identified, the most probable reasons are:
1. Arterial occlusion of the left superior labial artery due to intravascular product deposition.
2. Arterial spasm of the left superior labial artery due to trauma from the cannula.
D) Having identified the VO, how would you treat this patient?
This patient received immediate treatment to the lip body with 750 units of hyaluronidase (1500 units of Hyalase diluted in 1ml). After 30 minutes a second round of 750 units was given to the top lip, columella and nose tip. The hyaluronidase was administered using the serial puncture technique with a 32G needle. She was also prescribed a single dose of aspirin 300mg. Her capillary refill time in all areas was less than 2 seconds after the two rounds of hyaluronidase treatment.
She was followed up within 12 hours to reassess her capillary refill time, which remained normal. There was no skin breakdown so she did not have any post-VO medication prescribed. In cases of tissue breakdown, a course of antibiotics is advisable.
E) The patient also experienced blanching and duskiness at the tip of the nose. Anatomically, what could have caused this?
She is likely to have had a small embolus of filler occlude the left columella artery and therefore reduce blood flow to her nose. This may have occurred due to the initial injection of product or may have occurred after the first round of Hyalase was administered – breaking down an intravascular filler bolus with hyalase can cause micro emboli to progress distally along the artery and occlude smaller vessels. This is one of the reasons why careful follow up after a VO is necessary as ‘re-occlusion’ can occur.
Learn and practice your emergency protocols
The key takeaway from this vascular occlusion case study, is that you must learn and practice your emergency protocols. Understanding how to spot complications from lip filler or any other injectable treatment, then successfully manage them, is a vital skill for medical aesthetics professionals.
Our dedicated eLearning module Preventing and Managing Complications is available for all licensed medical aesthetic practitioners. It provides valuable, comprehensive support throughout your injecting career that acts as a handy reference tool.
Students who are currently taking, or plan to take our industry-leading Level 7 Diploma in Botox and Dermal Fillers now have this complications training included in their package as standard.
In order to be fully prepared for when a complication arises, print out your emergency protocol and place it somewhere easily accessible. Many injectors stick them to the inside of a cabinet along with their emergency supplies.
When you’re dealing with a complication, such as a vascular occlusion, it’s normal to feel nervous – particularly if it’s your first time. So, do yourself a favour now and make sure your protocols are printed in a large, easy to read font!
Remember to familiarise yourself with them regularly and practice them during downtime. When the time comes, you’ll be grateful you did.
All information correct at the time of publication. Article last fact-checked: 31 January 2023
Download our full prospectus
Browse all our injectables, dermal fillers and cosmetic dermatology courses in one document
By submitting this form, you agree to receive marketing about our products, events, promotions and exclusive content. Consent is not a condition of purchase, and no purchase is necessary. Message frequency varies. View our Privacy Policy and Terms & Conditions
Attend our FREE open evening
If you're not sure which course is right for you, let us help
Join us online or in-person at our free open evening to learn more
Our Partners















STAY INFORMED
Sign up to receive industry news, careers advice, special offers and information on Harley Academy courses and services

