How To Treat A Travelling Vascular Occlusion
Vascular occlusions (VOs) are most injectors’ worst nightmares even though they are fairly rare and can generally be easily treated. Recognising a VO is key. Would you know how to treat a travelling vascular occlusion, though? Or recognise one?
This topic came up as part of a complications discussion that took place between a new aesthetics practitioner and Harley Academy medical director, Dr Emily Mehta, on Comma (the Community for Medical Aesthetics).
Here we’ll run you through a brief overview of what a vascular event is, what an embolic vascular event is and how to treat one should it occur.
What is a vascular occlusion?
Essentially, a vascular occlusion is a blocked blood vessel, or vessels.
The Journal of Clinical and Aesthetic Dermatology published a paper on the Management of a Vascular Occlusion Associated with Cosmetic Injections in January 2020. This neatly sets out what a vascular occlusion is:
“A vascular occlusion occurs when blood is no longer able to pass through a blood vessel. It may be a complete occlusion or partial occlusion, resulting in a diminished blood supply. A vascular occlusion may be caused by an internal obstruction, such as a blood clot, a foreign body, such as filler material, or occur as a result of external compression. If left untreated, a vascular occlusion of a blood vessel supplying the skin can result in skin necrosis and tissue death.”
Treatment methods for vascular occlusions
Depending on the severity, vascular occlusions can be treated with:
- firm massage
- heat application
- tapping
- a combination of the above
- Hyalase (hyaluronidase).
Hyaluronidase, often referred to by its brand name: Hyalase, is a prescribed injectable enzyme which dissolves hyaluronic acid-based filler.
What is a travelling vascular occlusion?
In aesthetic medicine, a travelling vascular occlusion is a VO that presents remotely from the original injection site.
For example, this is the situation that was outlined in the aforementioned Comma discussion. It was an incident an injector had heard about and wanted to know how to treat in case it ever happened to her:
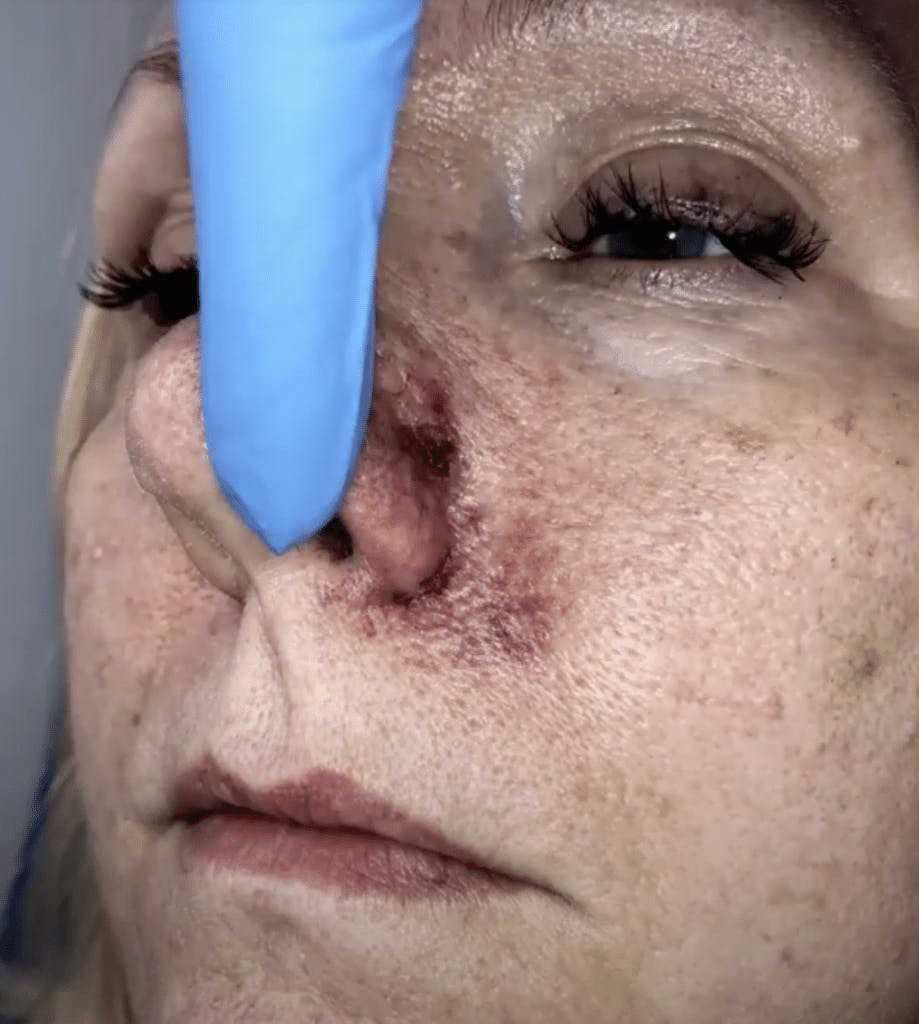
“The area injected with filler was the chin. Pustules and mottling were apparent on the lips and chin. Beneath the tongue a very aggressive looking ulcer appeared”.
How to treat a travelling vascular occlusion
Taking this Comma scenario as an example, let’s look at how to treat a travelling VO.
The question regarding the vascular complications that presented was, “In such a situation and the need to flood an area with Hyalase, if the VO has travelled to a different site to the injection site, would you inject Hyalase into the same area as you placed the filler?”

Dr Emily MacGregor advised:
“In order to place Hyalase correctly you need to use the skin changes to work out which vessels have been occluded and administer Hyalase in that area in the correct plane, remembering that intra-vascular filler can embolise and occlude a vessel away from the site of injection.
“In this example it sounds like the ascending mental artery (AMA) has been occluded and emboli have also affected the sublingual – supplying the floor of the mouth – and the inferior labial (ILA). All three can be connected via anastomoses, although this is quite rare from what I’ve read.
“Hyalasing the AMA involves placing the product deep throughout the chin. For the ILA, I would use a cannula deep in the lip but the challenging one is the sublingual. I haven’t heard of this being targeted with Hyalase before but just using anatomy, I think to reach it you would need to inject behind the chin between the mandible and hyoid bone – something I hope I never have to do! Personally I wouldn’t want to inject through the floor of the mouth and through an ulcer.
“The key point in all of this isn’t to learn crazy techniques to reach every arterial branch but to spot the occlusion more quickly – “an aggressive looking ulcer” means that perfusion wasn’t restored quickly enough.”
The injector revealed that the scenario had been resolved by administering Hyalase at the chin within 24 hours of the initial treatment, then again within 48 hours. Deeper Hyalase was given 72 hours later.
She added, “I understand the patient is recovering but has been seen by an ENT specialist and has been advised she’ll have severe scarring beneath the tongue.”
Preventing Vascular Occlusion
In addition to understanding how to spot and treat VOs, it is of vital importance to know how to minimise the risk of them occurring in the first place.
For advice on this from expert injectors, we suggest reading our article on Preventing Filler Embolus and Vascular Occlusion.
Additionally, once you are confident in your injecting technique, we recommend learning how to use a cannula. This method has been shown to make VOs less likely.
For hands-on guidance on getting your cannula technique up to scratch, a one-to-one training session can be immensely beneficial. Harley Academy offers tailored 1:1 Training in Mid-Face and Cannula to help you really get to grips with this way of working.
So, whether you are new to this method or just want to perfect your approach, this expert guidance and one-to-one attention can really help improve your practice – as well as potentially helping you to avoid any nasty vascular occlusions!
All information correct at the time of publication
Download our full prospectus
Browse all our injectables, dermal fillers and cosmetic dermatology courses in one document
By submitting this form, you agree to receive marketing about our products, events, promotions and exclusive content. Consent is not a condition of purchase, and no purchase is necessary. Message frequency varies. View our Privacy Policy and Terms & Conditions
Attend our FREE open evening
If you're not sure which course is right for you, let us help
Join us online or in-person at our free open evening to learn more
Our Partners















STAY INFORMED
Sign up to receive industry news, careers advice, special offers and information on Harley Academy courses and services

