How To Prevent And Manage Filler Migration
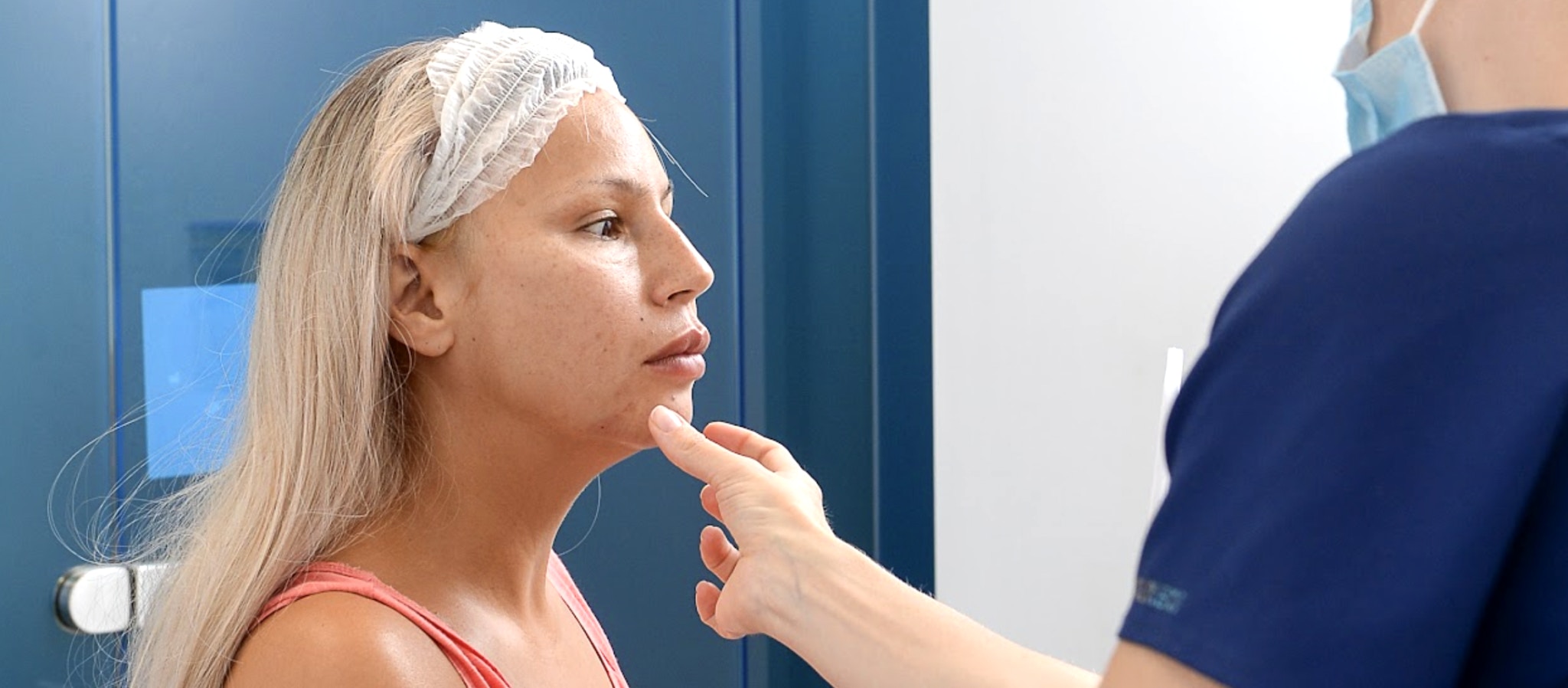
Filler migration is a common effect of dermal fillers, which are used in facial aesthetic treatments.
Though safe when administered by licensed practitioners, fillers, like all aesthetic treatments, carry the risk of adverse effects and complications.
A recent study on filler migration highlights the risks of unwanted side effects from filler injections. This was undertaken by a team from Brazil and published in the Cosmetics journal.
We speak to Dr Kalpna Pindolia about its findings. She also explains the crucial information all injectors need to know about filler migration, including how to prevent and correct it.
Dr Kal is the Education Director at Harley Academy and an experienced aesthetic medicine specialist. She currently also practises at STORY clinic in Marylebone.
What is the most common region for filler migration?
The paper notes, injections into the nose, lips, nasolabial folds, and forehead, including the glabella, are more often reported for filler migration. We asked Dr Kal if this is accurate in her opinion?
She explains, “The inclusion criteria for this study was observational studies, case reports, and clinical trials. So, it should include a breadth of reported cases for hyaluronic acid filler and polyalkylimide. However, unreported cases and cases of migration which are subclinical or not perceived by patients, would not have been represented.”
“My experience is mainly with hyaluronic acid filler. Most cases of migration I have seen were from lip filler and filler in the under eye region.”
Why do we see filler migration in some areas more than others?
“Baseline anatomy is a big consideration in filler migration,”says Dr Kal. She clarifies that this is due to the fact that “filler tracks through the path of least resistance. Mobile areas of the face are also particularly prone to movement of product.”
“This is why lips often present with migrated filler. They are a small, mobile area, and easy to overfill either in one sitting or over time.”
But it’s not just mobile areas. She counsels that “technique can also contribute. For example, cannulas are thought to cause more backflow of filler. There is evidence to suggest needle size, angle of insertion and injection speed also contribute to the risk of filler movement.”
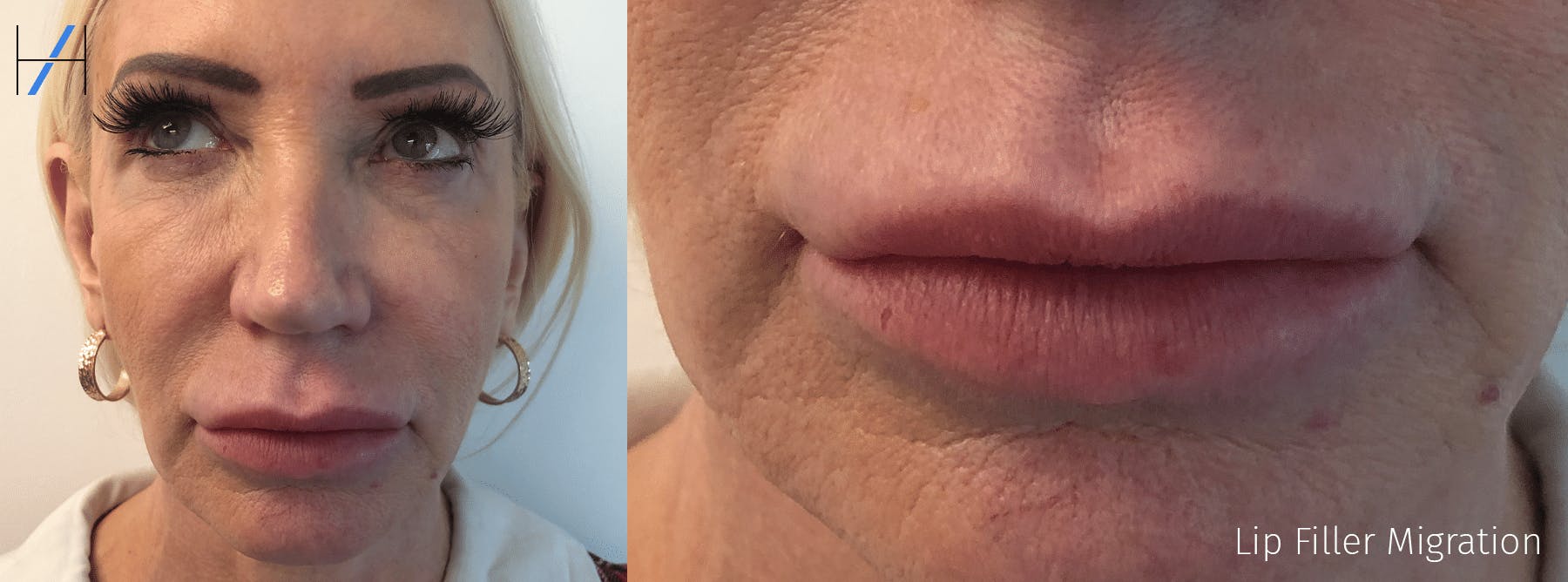
What can aesthetics practitioners do to limit the chance of migration?
Dr Kal notes, “One crucial factor is knowing when not to treat.”
“Apart from inspecting the treatment area from different angles and in motion, also palpate the area. This is to get a sense of the volume already placed.”
She cautions, “Over-treatment or repeated treatments can lead to the appearance of migrated filler.”
Lastly, “understand your product rheology. Keep injected volume as low as possible and keep the extrusion force on your product as low as possible. This is so that the injection pressure is not too high, reducing the risk of filler migration.”
What are the best ways to deal with filler migration?
First you need to know what you’re looking for. An early sign of filler migration is “swelling of the region, which becomes more distinct and easily palpable over time.”
When it comes to the best ways to manage this migration, Dr Kal states, “there are two options.”
Conservative management approaches
She explains that “conservative management would mean leaving the filler to dissolve naturally. Theoretically, regular massage and warm compresses could also aid the process.”
“However, in my experience, the longer migrated filler is left, the less likely this option will lead to the desired resolution,” she warns.”This is especially true many months post treatment.”
“Evidence is increasingly suggesting that filler may stay in situ for much longer than previously thought.”
Dissolving filler that’s migrated
“The second option is using hyaluronidase to break down the filler in the area affected,” explains Dr Kal. “This is quick and effective if the patient has no contraindications for treatment.”

What are some common mistakes new practitioners make when dealing with this?
Dr Kal states that there are a few mistakes that can typically occur in this situation.
“The most common mistake is not noticing the filler migration in the first place. New practitioners may not pick up on the more subtle signs. Then if they do notice, and migration is obvious, it’s also a delicate conversation to have with a patient. This is especially true if the patient has not noticed it themselves, which can often be the case.”
“The other mistake is treating migration too early. Sometimes as swelling post treatment subsides, any presumed migration may settle,” she notes.
“Due to lack of experience, occasionally, they may fail to consider other differential diagnoses as well, such as inflammatory nodules.”
Learning how to prevent and manage filler complications
Safe administration of individual filler treatments is taught on all our injectables training courses. These are open to doctors, dentists and nurses.
Our Level 7 Diploma in Botox & Dermal Fillers is a Master’s level course that will boost your confidence and understanding on a deeper level. By teaching you the science, theory and practice of injectable treatments, you’ll learn how to administer injectables in line with the Health Education England’s (HEE) Qualification Requirements for Delivery of Cosmetic Procedures. These HEE guidelines are the starting point for conversations regarding licensing scheme proposals for England.
For dedicated learning on this topic, choose our Preventing and Managing Dermal Filler Complications online course. This uses real-life case studies to explain how to prevent, identify and manage complications. This forms part of our Level 7 course but is also available to purchase separately.
For more information on our range of medical aesthetics training courses, reach out to our Courses team. Book a call to receive personalised advice on finding the best aesthetic medicine education for you.
All information correct at the time of publication
Download our full prospectus
Browse all our injectables, dermal fillers and cosmetic dermatology courses in one document
By submitting this form, you agree to receive marketing about our products, events, promotions and exclusive content. Consent is not a condition of purchase, and no purchase is necessary. Message frequency varies. View our Privacy Policy and Terms & Conditions
Attend our FREE open evening
If you're not sure which course is right for you, let us help
Join us online or in-person at our free open evening to learn more
Our Partners















STAY INFORMED
Sign up to receive industry news, careers advice, special offers and information on Harley Academy courses and services

