Exploring Non-Ischaemic Dermal Filler Complications
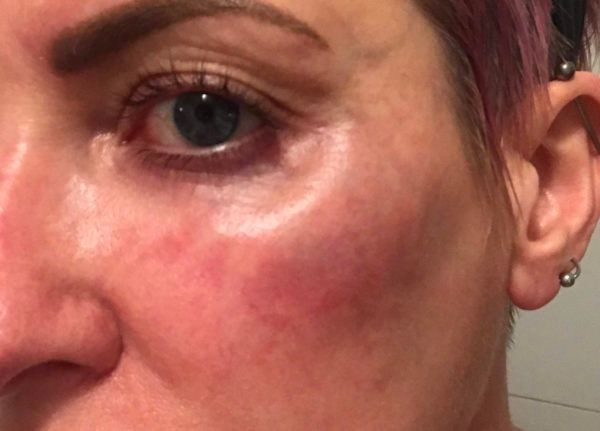
As the use of dermal fillers grows, so does the incidence of non-ischaemic complications. As with any treatment in aesthetic medicine, adverse events are always a possibility.
A recent study published in the Plastic and Aesthetic Research journal explores a range of complications that span bruising and oedema, to more complex conditions. These include delayed hypersensitivity nodules and biofilms.
Compiled by a team of researchers in California, USA, the study reviews the causes of various non-ischaemic complications. It discusses their risk factor and reviews management and prevention techniques.
This article discusses the findings. These should always be interpreted using critical appraisal to consider the relevance of the findings to your clinical practice.
DERMAL FILLER COMPLICATIONS
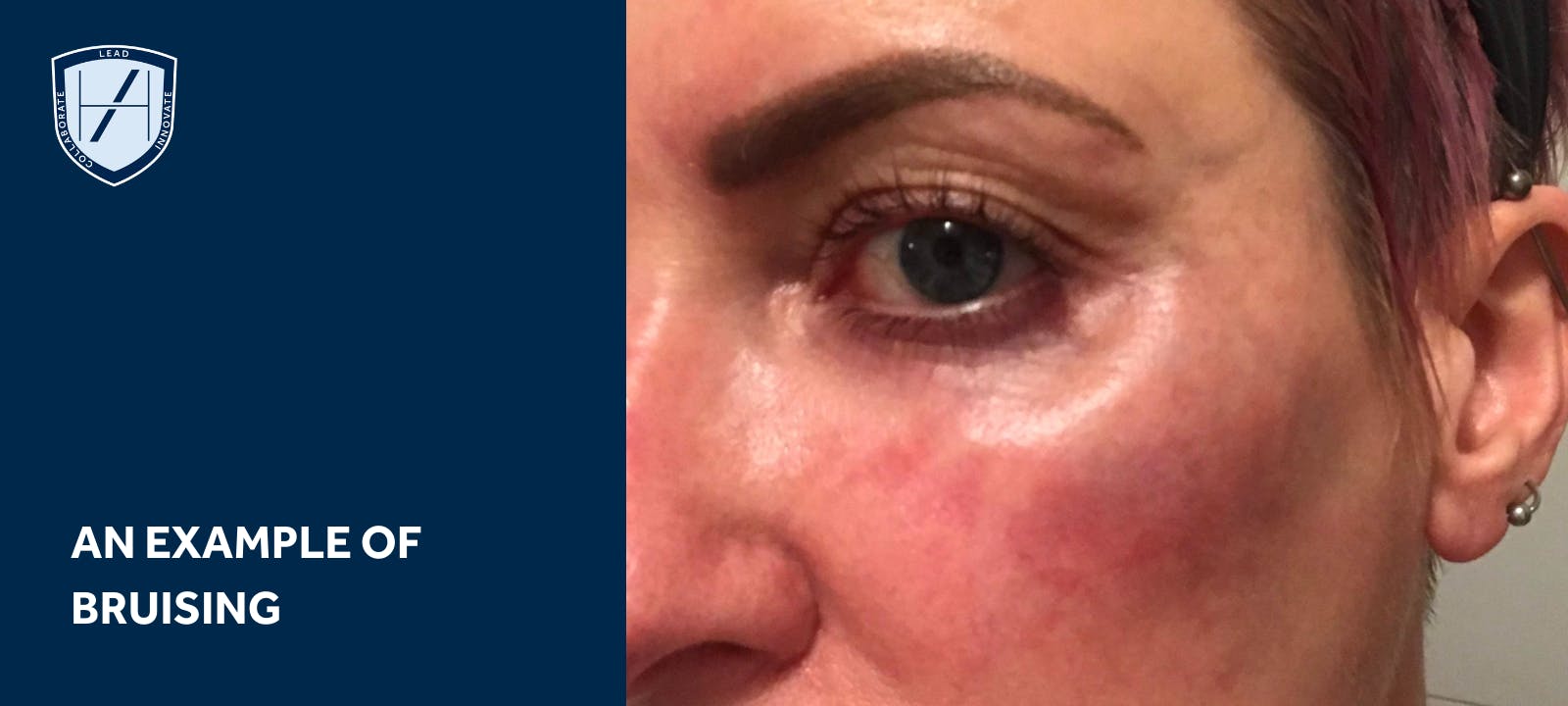
Bruising
Bruising is most often seen after filler injections, secondary to needle-associated perforation or vessel rupture from trauma in the area.
Study authors advise the “most common location is the perioral rhytid, lower eyelids, the upper third of the nasolabial fold, upper lip and lateral edge of the lower lip.”
The bruising will darken for a day and resolve in 5 to 10 days with minimal effect on the aesthetic results. They also state that “bruising is generally managed by applying immediate pressure and ice packs, both during and after the injections.”
It has been suggested that Vitamin K oxide gel can be used to help reduce the severity of bruising. However this is based on research conducted after laser treatment.
Patients on anti-inflammatory or anticoagulation medications may be at an increased risk of bruising. As always, it’s recommended to perform a thorough consultation with patients assessing any contraindications and evaluating the risk of stopping said medication. “If deemed appropriate, non essential medications with anticoagulation effects may be paused one week prior to injection” the research advises.
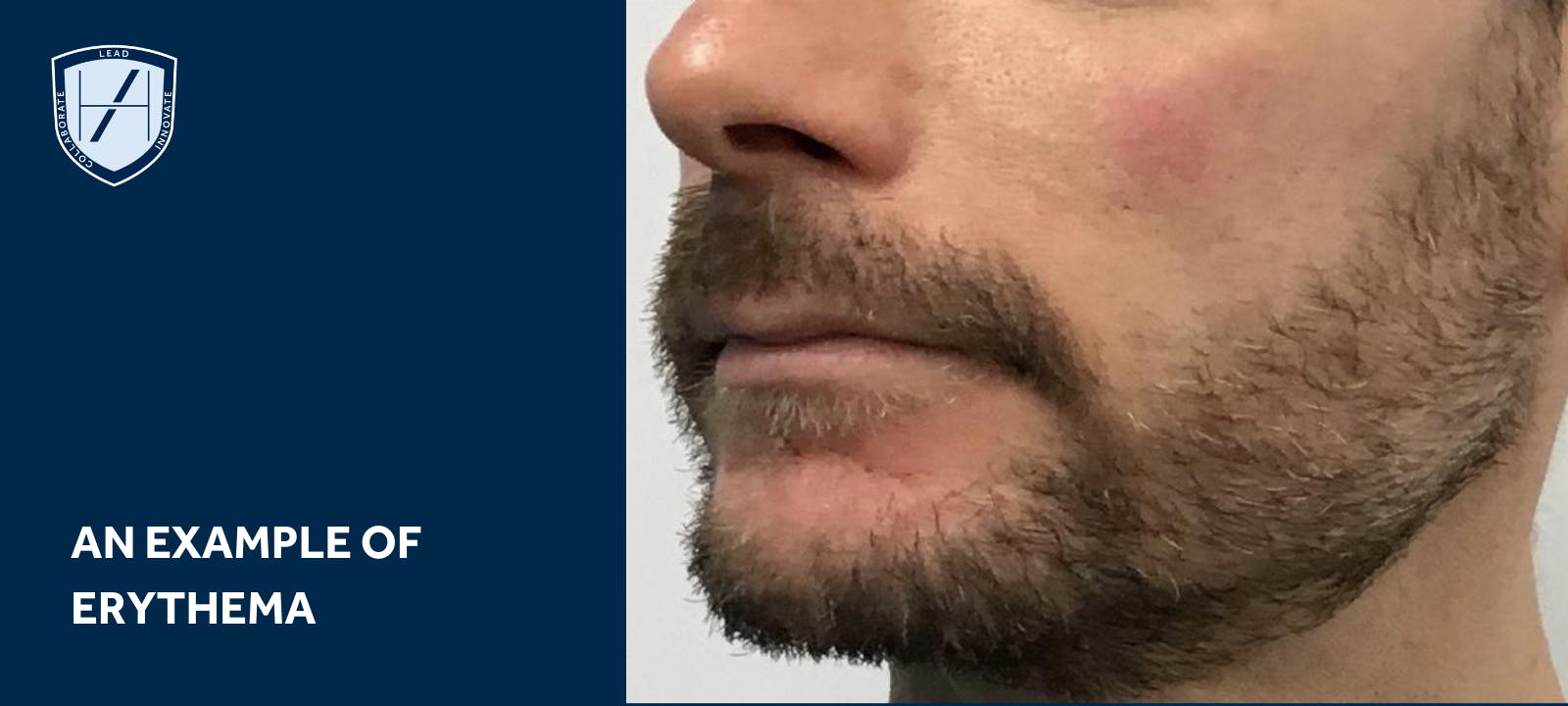
Erythema
Another non-ischaemic dermal filler complication is erythema. This comes secondary to puncture trauma and inflammation. Similar to bruising, firm pressure and ice packs during and after injection can help.
Erythema tends to resolve within a couple of hours. Always inform the patient of this possible side effect.
Oedema
The third most common problem is oedema. Similar to bruising, firm pressure and ice packs during and after injection can help.
A blunt tip cannula has been shown to produce less oedema, pain and bruising at the injection site with faster recovery times.
Oedema can take up to a week to resolve and the most frequent areas it occurs in are the lips and periorbital region.
It tends to be worse in the mornings after the patient wakes up and gradually improves throughout the day. As the study states, “this cycle tends to repeat itself daily until it all resolves in 5-10 days.”
It’s worth noting that shorter-chain hyaluronic acids (HA) have a higher tendency to cause inflammation upon injection. This can cause increased oedema. More severe or prolonged forms of oedema include angioedema and malar oedema. Keep reading for more about these types of filler complications...
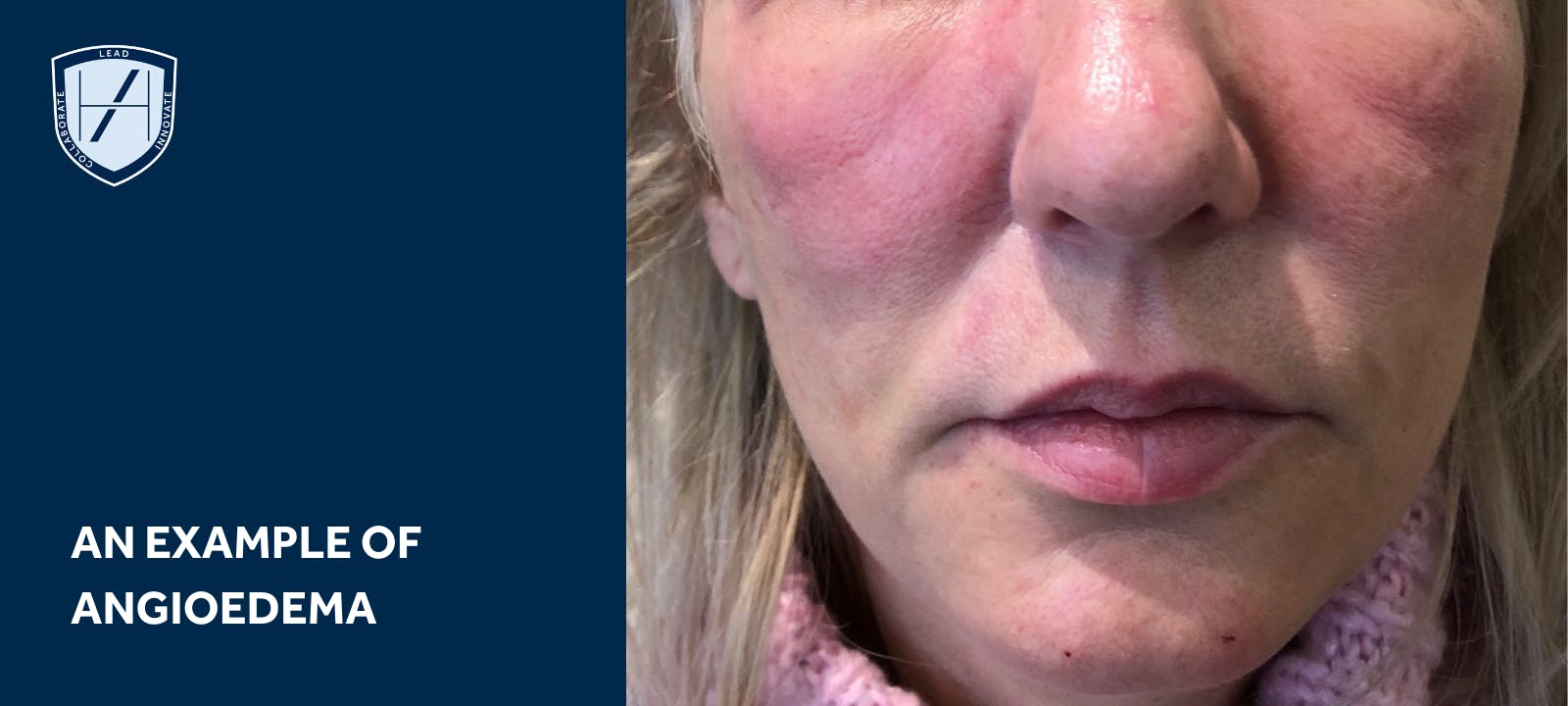
Angioedema
Next up there’s angioedema, a non-ischaemic filler complication which “occurs due to Type I hypersensitivity response to dermal fillers.” The release of immunoglobulin E (IgE), a B cell response, degranulates mast cells. This causes a classic triad of swelling, oedema and itching associated with an allergic response.
Fillers are essentially foreign bodies, however hyaluronic acid fillers are considered less immunogenic compared to bovine collagen fillers.
Angioedema can occur within hours, lasting up to 3 to 7 days. Rapidly progressing oedema has the potential to cause airway obstruction.
The authors suggest that for “resistant or persistent oedema, oral prednisone, cortisone tables, or injections can be considered for treatment.”
If the oedema lasts more than 6 weeks, it’s classified as chronic angioedema. This can be managed with non-sedating and sedating antihistamines, before moving onto oral steroids or immunosuppressants.
Malar oedema
Malar oedema is frequently reported after tear trough, infraorbital hollow and lid/cheek junction area filler injections. “It’s defined as a collection of fluid over the malar eminence below the level of the infraorbital rim.”
The authors note that a “recent study found an incidence of approximately 11% for malar oedema following periorbital filler injection”. It confirmed older patients with thinner skin are at higher risk.
In the study, researchers explain “the malar fat pad is a triangular-shaped area of subcutaneous fat based at the nasolabial fold with its apex at the malar eminence.”
It’s recommended to inject filler directly on the periosteum within the boundaries of the malar septum. Place small boluses of filler directly on the bone.
There’s two things to note in patients who experience malar oedema. First is differentiating malar oedema from orbital fat prolapse. Orbital fat prolapse tends to present more eminently than malar oedema and would require different management.
Patients who have pre-existing malar oedema should also be counselled that receiving tear trough filler could worsen this. In some patients the malar oedema may not resolve and they should avoid tear trough filler injections entirely.
You can manage this filler complication through head elevation, cool compresses, manual lymphatic compression, hyaluronidase, and methylprednisolone for HA fillers.
In one study of 19 patients with malar oedema, an injection of 15-30 U/cm of hyaluronidase appeared to be sufficient to resolve oedema for 15 patients.

Paraesthesia/nerve injury
Paraesthesia, also known as nerve injury, is a rare filler complication that occurs from direct trauma from the needle or injection into the nerve, or tissue compression.
Research suggests that the most common area of nerve damage is the infraorbital nerve, occurring more frequently if the intraoral approach is used. The nerve damage can be transient to permanent.
The authors of the study suggest the best way to avoid this is to be aware of the anatomy and neurovascular bundles around the injection site.
Treatment with “triamcinolone at the infraorbital foramen as well as breaking up the material with lidocaine or saline” is recommended.
ADDITIONAL FILLER COMPLICATIONS
Other dermal filler complications discussed within the study include:
Skin discoloration
This covers neovascularization, hyperpigmentation and blue-grey dyschromia.
Nodules and Biofilms
Divided into non-inflammatory and inflammatory categories, this includes infection, herpes reactivation and delayed hypersensitivity nodules.
Delayed hypersensitivity reactions
Specifically, this explores studies into Vycross fillers, flu-like illness and Covid-19.
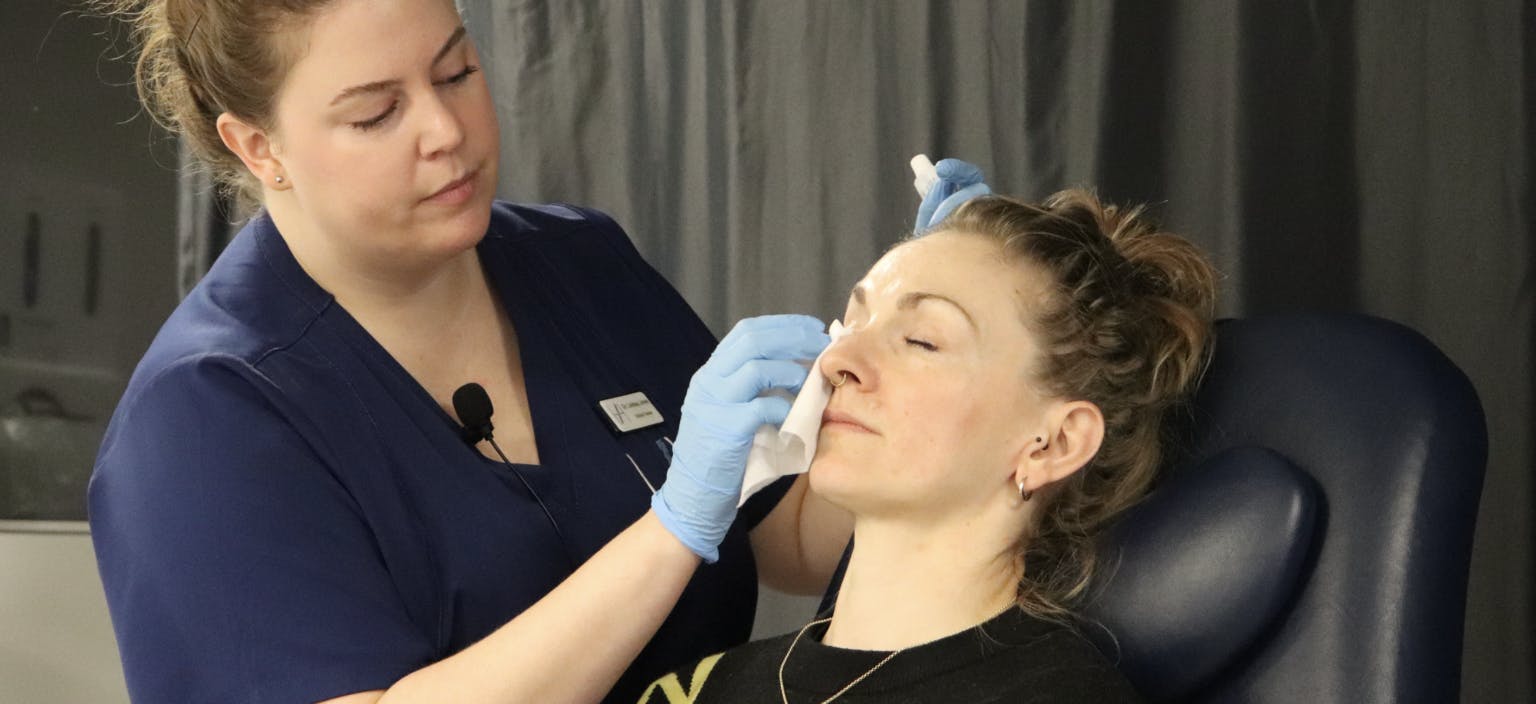
Prevention is key for avoiding filler complications
Complications have the potential to affect a patient’s care and results. Prevention is an important consideration when it comes to managing dermal filler complications.
The study recommends a number of measures to prevent or minimise the risk of dermal filler complications. These include:
1. Assess for an contraindications
2. Ensuring the face is cleaned properly before injecting
3. Using aseptic technique
4. Consider injection technique
5. Deliver post-treatment care information.
Learn how to prevent and manage filler complications
Safe administration of filler treatments is taught on our injectables training courses. These are open to registered doctors, dentists and nurses.
For more information on this subject, check out our online course Preventing and Managing Dermal Filler Complications.
This eLearning course is included free of charge in our Level 7 Diploma in Botox & Dermal Fillers. The Level 7 is a Master’s level, JCCP-approved course that will boost your confidence and understanding of injectables.
For more information on our range of medical aesthetics training courses, reach out to our Courses team. Book a call to receive personalised advice on finding the best aesthetic medicine education for you.
All information correct at the time of publication
Download our full prospectus
Browse all our injectables, dermal fillers and cosmetic dermatology courses in one document
By submitting this form, you agree to receive marketing about our products, events, promotions and exclusive content. Consent is not a condition of purchase, and no purchase is necessary. Message frequency varies. View our Privacy Policy and Terms & Conditions
Attend our FREE open evening
If you're not sure which course is right for you, let us help
Join us online or in-person at our free open evening to learn more
Our Partners















STAY INFORMED
Sign up to receive industry news, careers advice, special offers and information on Harley Academy courses and services

